Medical science has misunderstood obesity for decades. It's not the cause of insulin resistance. It's the result. Learn how seed oils contribute, as described in my Energy Model of Insulin Resistance, published in Frontiers in Nutrition Science.

Cholesterol Is Good, The American Heart Association is Bad
Table of Contents
- Cholesterol is Not the Cause of Heart Attacks
- Keys’ First Tactic was to Blind Doctors With Science
- Keys also convinced doctors in the AHA to accept funding from companies selling vegetable oil-based shortening.
- Keys Helped Design a Study to Test the Effects of a High-PUFA Diet
- The Minnesota Coronary Experiment Stacked the Dietary Deck in Favor of PUFA
- The BIG Question: Does a High-PUFA, Cholesterol-Lowering Diet Reduce Mortality?
- PUFAs Increase Mortality
- To Hide the Facts About Fat the AHA and Keys Hid Smoking Data for 25 Years
- Why Single Out Ancel Keys?
- Related Content on DrCate.com:
The American Heart Association Started Calling Cholesterol Bad When Companies Using Vegetable Oils Started Making Donations
Today I want to make it clear that, if you’ve adapted a low-PUFA lifestyle (PUFA=PolyUnsaturated Fatty Acid) and your cholesterol has gone up, it’s actually a good thing in spite of what the AHA says. I wrote this post originally in 2016, but updated it in 2020 to better drive home these key takeaways and help dispel the fears many of us have from seeing our own cholesterol numbers, especially LDL cholesterol, climb:
- The American Heart Association recommends consuming “more vegetable oil” because it’s low in saturated fat and high in polyunsaturated fat (PUFA) and shows no concern that we’re already consuming historically high amounts of both vegetable oil and PUFA.
- The AHA’s has failed to publish the available evidence that consuming these oxidation-prone oils at current levels is radically harmful to our health in any of their dozen or so professional journals.
- It’s clear that PUFA consumption reduces blood cholesterol, but what’s less clear is why this happens.
- There are many reasons to conclude that eating enough PUFA to lower cholesterol is terrifically harmful to your health.
- The best study ever designed to test the idea that PUFAs are healthy ultimately showed that they were unhealthy, so the study authors didn’t publish it.
- This is scientific fraud.
- The AHA has been engaging in scientific deception around saturated fat, cholesterol and PUFAs for decades.
- Doctors who dispense the American Heart Association’s dietary advice are doing more harm than they know.
Cholesterol is Not the Cause of Heart Attacks
When your primary care doctor recommends cutting out foods like butter and eggs in favor of Smart Balance and egg beaters, or your naturopathic doctor tells you cow’s milk is unhealthy because of saturated fat and you’d be better off with rice milk, when your trainer tells you to eat skinless boneless chicken breast and protein powders, when your McDonald’s fries are soaked in seed oils instead of beef tallow, and your take out pizza is made with soy oil instead of olive oil, it’s important to realize that all these changes are taking the freshness and realness of your diet down a notch or two—and some of these newer alternatives are outright toxic.
Nobody would want these lower-quality processed foods were it not for the idea that saturated fat and cholesterol clog your arteries. This idea has made us afraid of the very foods our bodies need the most, and it’s enabled the processed food industry to thrive as never before. The saturated fat lie helped to create a demand for alternative fats that come from soy, corn, and other subsidized monoculture crops soaked in pesticides and herbicides, destroying the soil and with it our ability to live sustainably off the land.
The myth that saturated fat and cholesterol clog arteries has acted like a virus, a contagious idea that infected humanity’s relationship with food and separated us from thousands of years of culinary tradition and farming wisdom. It has allowed for the painting of all animal products with one brush, as if how they’re fed and raised makes no difference, putting thousands of traditional family farms out of business. Instead of being raised by farmers who treat their animals like family, most cattle, pork, and poultry are now subjected to horrific treatment in industrial-scale agricultural operations. This is affecting farmers and people who love animals, certainly, but it also affects all of us because it means poultry, pork, and beef all taste worse and are far less nutritious.
This article is continued below...(scroll down)
This one idea, that saturated fat, and cholesterol cause heart disease, has gradually turned us against nature, the source of human health. To really get comfortable with the fact that cholesterol is not your enemy and vegetable oils are, it’s helpful to understand the history of this idea.
Its origins can be traced back to an influential figure in the American Heart Association, named Ancel Keys.
Ancel Keys’ Sold the American Heart Association’s Soul for $1.7 Million
As I wrote in Chapter 7 of Deep Nutrition, called Good Fats and Bad, it all began back in the 1950s and 1960s, when an oceanographer and eel physiologist named Ancel Keys designed a series of highly influential experiments that forever altered the course of American dietary history. Keys had a powerful personality, which he used to influence the American Heart Association leadership. As a result, a deal was brokered where Proctor & Gamble, makers of hydrogenated vegetable oil, paid the AHA 1.7 million dollars.
Before Keys, Americans enjoyed traditional foods like butter, eggs, and bacon without worrying about their health. After Keys made the cover of Time Magazine on Jan 13, 1961, the American public was introduced to the idea that saturated fats were clogging their arteries. That idea ultimately led to a sea change in the foods we eat. Real fats would increasingly be replaced by factory-made seed oils, and the era of chronic disease would begin.
This article extends the arguments I made in Deep Nutrition to show how Keys and his allies misled doctors and hid the results of their own studies that would have proved them wrong.
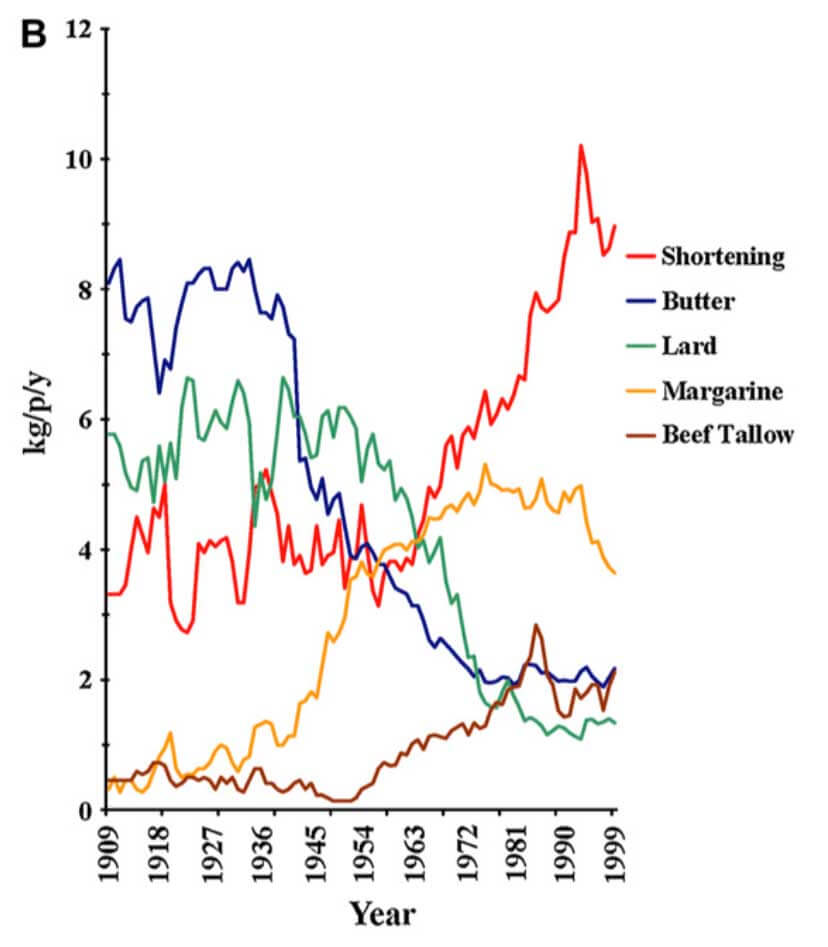
Keys’ First Tactic was to Blind Doctors With Science
In the 1961 Time magazine article celebrating Keys, he is quoted as warning us that “Americans eat too much fat. With meat, milk, butter, and ice cream, the calorie-heavy U.S. diet is 40% fat, and most of that is saturated fat—the insidious kind…that increases blood cholesterol, damages arteries, and leads to coronary disease.”
During interviews like these where Keys discussed his research and experiments, he led the audience to believe that saturated fat from butter and eggs caused atherosclerosis. But during those interviews, he was not being completely honest. Had he been, he would have said that his studies showed margarine caused atherosclerosis. The margarine in his experiments contained saturated fats that had been artificially created from vegetable oils using a process called hydrogenation. Hydrogenated vegetable oils contain not just saturated fat but also trans fat and a whole host of other unnatural molecules. Trans fat is now known to have a multitude of toxic effects on the body, causing fatty liver, weight gain, as well as lead to heart attacks and stroke. It’s so unhealthy that cities like Manhattan and San Francisco have outlawed its use in restaurants.
Keys didn’t have to work very hard to hide this deception. One publication he authored entitled “Hydrogenated fats in the diet and lipids in the serum of man” should have been a red flag that he was not using real food in his experiments. But few recognized it as a red flag because few were conversant with the terms he was using. Although doctors do learn some biochemistry, food-processing terms like hydrogenation would not become part of the standard curriculum until 50 years after Keys, nearly a century after they were introduced into the food supply.
Keys also played games with statistics. Most notoriously, he cherry-picked data points that made it look like countries that ate the most fat also had the most heart attacks. In other words, he excluded countries that ate a lot of fat but had few heart attack deaths and vice versa. The details of this historic deception have been covered by many researchers including Dr. Uffe Ravnskoff, Dr. Malcolm Kendrick, journalist Nina Teicholz, and myself.
What’s less well known is that Keys also compiled smoking data starting in 1958 at the beginning of the Seven Country’s Study, but he failed to publish the smoking until 1980, well after he had successfully deluded Americans into believing saturated fat clogged arteries.
Keys was the first person to collect large amounts of data on the relationship between smoking and heart attacks. But Keys never talked about the smoking data he collected, and what was a very clear and very strong correlation between cigarette smoking and heart attacks wasn’t published until many years after the initial data was collected.
But by then, it was too late. The saturated-fat cat was out of the bag and nobody in any position of authority was willing or able to put it back in. The belief that saturated fat is unhealthy because it elevates cholesterol, which supposedly clogs our arteries and causes heart attacks and stores, now forms the basic foundation of most nutrition science in spite of the fact that it was based on a series of deceptions and scientific half-truths.
Fortunately, blockbuster books like Good Calories, Bad Calories, The Big Fat Surprise, and The Primal Blueprint, as well as my own books, have gone a long way towards informing the reading public on the health harms of hydrogenated vegetable oils, and the lack of harm from natural saturated fat. This information has trickled down to influence the thinking of some doctors as well, and a few have lifted their restrictions on butter and eggs.
But Keys did more than fool physicians into believing eating butter and eggs would kill us.
Keys also convinced doctors in the AHA to accept funding from companies selling vegetable oil-based shortening.
Keys was a major fundraiser for the American Heart Association and a close associate of their medical leadership, most notably Paul Dudley White, who famously treated President Eisenhauer after his first of several heart attacks. Dr. White was not initially in step with Keys about the idea that saturated fat causes heart attacks, but soon after they met he changed his opinion. That flip-flop was perhaps an outgrowth of the need for corporate sponsorships for the American Heart Association, which Dr. White directed for several years.
As Nina Teiholz writes in The Wall Street Journal, “In 1948, P&G made the AHA the beneficiary of the popular ‘Walking Man’ radio contest, which the company sponsored. The show raised $1.7 million for the group and transformed it (according to the AHA’s official history) from a small, underfunded professional society into the powerhouse that it remains today.”
It’s possible that Keys brokered the deal, but that is a question that for now remains unanswered. The fact is, the AHA was clearly in bed with the biggest vegetable-oil company in the world at the time and Keys’ linguistic tricks and statistical deceptions made Procter & Gamble’s product look healthier than their only competition at the time, the traditional fats like butter, tallow, and lard. It’s entirely possible that Keys at one point in his career truly believed that traditional fats like butter, tallow, and lard caused heart attacks. But once his reputation became dependent on the idea, he crossed a line. The next section discusses what I think is the worst example of how Keys’ and the AHA’s medical leadership worked together in an attempt to make vegetable oil look healthy.

Keys Helped Design a Study to Test the Effects of a High-PUFA Diet
In the 1960s, Ancel Keys and the president of the Minnesota chapter of the AHA, Dr. Ivan Frantz, designed one of the largest, most rigorous experiments ever conducted to test an important question: how do vegetable oils affect our health. Called The Minnesota Coronary Experiment (MCE), it was the highest-quality kind of study, a double-blind randomized controlled trial. And it was huge, a massive undertaking involving thousands of adult residents of six state mental hospitals and one nursing home, where inmates had no choice but to eat what was put in front of them and so compliance with the experimental diets was practically guaranteed. Everything was done to assure the that results were going to be about as reliable and meaningful as possible.
The study was composed of two parts, designed to test the validity of two different hypotheses:
1) That a diet high in polyunsaturated fat from vegetable oils would lower cholesterol.
2) That this reduction in cholesterol levels would prevent atherosclerosis and deaths from heart attack and stroke.
Both hypotheses are important, but number two is even more important because if PUFAs do in fact lower cholesterol but this fails to translate to a reduction in heart attacks and strokes, this challenges the idea that cholesterol is the cause of heart attacks.
To test the two hypotheses, the study subjects were divided into two groups and fed two different diets for at least a year. One diet, called the control, was intended to mimic the typical American’s diet and was relatively high in saturated fat. The other, called the experimental diet, was low in saturated fat and high in polyunsaturated fat from corn oil.
The Minnesota Coronary Experiment Stacked the Dietary Deck in Favor of PUFA
The experimental, high polyunsaturated-fat diet contained lean meats “filled” with vegetable oil (called “filled meats”), skim milk, and cheeses to which corn or other vegetable oils were added, along with some margarine—no butter or natural animal fats. But the so-called control diet was not exactly what most Americans at the time would eat. Rather than containing butter and animal fats, it was full of margarine and shortening as these are also rich sources of saturated fats.
What’s key here is that this so-called control diet contained substantial quantities of trans fat. In other words, the experimental diet was being compared to a very unhealthy diet, not a true control. What was in fact being examined was not the effect of saturated fat versus PUFA but, rather, the effect of trans fat plus saturated fat from hydrogenated oils versus PUFA. By comparing PUFA to unnatural factory foods, Keys stacked the deck in favor of PUFA. Given that Keys had been studying trans fat’s effects for years before this study started, I doubt this little cheat was accidental.
Even with this deck stacking, real science would make an appearance in the form of meaningful results that were not what the researchers were hoping to see.
Part 1, Question 1) Do PUFAs Lower Cholesterol?
Answer: Yes!
Both the control and study groups had their cholesterol levels tested at the onset of their participation in the study and again one year later. In the beginning, the numbers were very well matched and nearly identical. One year later, the high-PUFA diet group had cholesterol levels 30 points lower, on average, than those in the so-called control group. This was not an entirely new finding since many other less well designed studies and animal experiments had already demonstrated that PUFAs reduce cholesterol.
It’s important to know that this predictable reduction in cholesterol is the American Heart Association’s justification for recommending vegetable oils. That’s why products like Smart Balance and thousands of other high-PUFA products claim to be “heart-healthy.”
But here’s the problem: we’ve never shown that lowering cholesterol by eating more PUFAs prevents heart attacks. That’s the question that part 2 of the study was designed to test.
Part 2, Question 2) Do PUFAs Prevent Heart Attacks?
Answer: Inconclusive.
Both groups were followed for an average of 3 1/2 years, or until their deaths. Participants needed to have been on the diet for at least one year before death for the result to be counted. Upon dying, an autopsy was performed to determine the cause of death. While they gathered all the data that would have answered the second question, and almost certainly were aware of what it showed, they simply never published it. Fortunately, the lead scientist, Dr. Frantz, left most of the data, some 2355 medical charts and 149 completed autopsy files crammed into dusty boxes, undisturbed in his basement.
Some 30 years later, Christopher E. Ramsden, described as the Indiana Jones of medical research, gained access to what remained of the raw data. Most of it was there, but many of the autopsy reports necessary to determine the cause of death were missing. That meant the remaining data couldn’t definitively answer the question about heart attacks. But there was enough data to determine how many people in each group died, which is a very important question.
The BIG Question: Does a High-PUFA, Cholesterol-Lowering Diet Reduce Mortality?
Answer: No.
That’s kind of the point, right? Not dying? Even if the diet reduces deaths from heart attacks, if it increases deaths from other conditions, we’d need to know that before making any recommendations to include PUFAs in our diet. So the mortality question is the BIG question that needed to be addressed.
As Dr. Ramsden writes in his landmark article Re-evaluation of the traditional diet-heart hypothesis: analysis of recovered data from Minnesota Coronary Experiment (1968-73). “The number, proportion, and probability of death increased as serum cholesterol decreased.” In other words, the more a person’s cholesterol dropped, the more likely they were to die. For each 30 mg/dL reduction in serum cholesterol, the risk of death increased by 22%. Ramsden said in an interview that “[w]e were able to find that actually those that lowered their cholesterol more actually had increased rather than reduced risk of death,” adding, “It was surprising.”
If this data is valid, it’s more than a surprise. It’s kind of a big deal. Actually, it’s an outrageously big deal. Why wasn’t this information published as soon as it was available? According to the lead author’s son (interviewed by Malcolm Gladwell for a podcast called The Basement Files), these results were so shocking to Dr. Frantz, he didn’t know what to make of it all and simply “couldn’t bring himself to publish them.”
Some suggest we should let these guys off the hook, rationalizing that it wasn’t self-interest holding them back; it was self-doubt. It’s human nature for researchers to doubt their results when the results are unexpected.
But I’m not making excuses for these two icons of nutrition science whose careers would have been dramatically altered by results that proved them wrong. They may have had some interest in nutrition science, but I reckon they were also interested in money. By failing to show their results, that PUFAs kill people more often than deadly trans fat, they protected the American Heart Association’s chief source of funding, which was at that time the seed oil industry.
PUFAs Increase Mortality
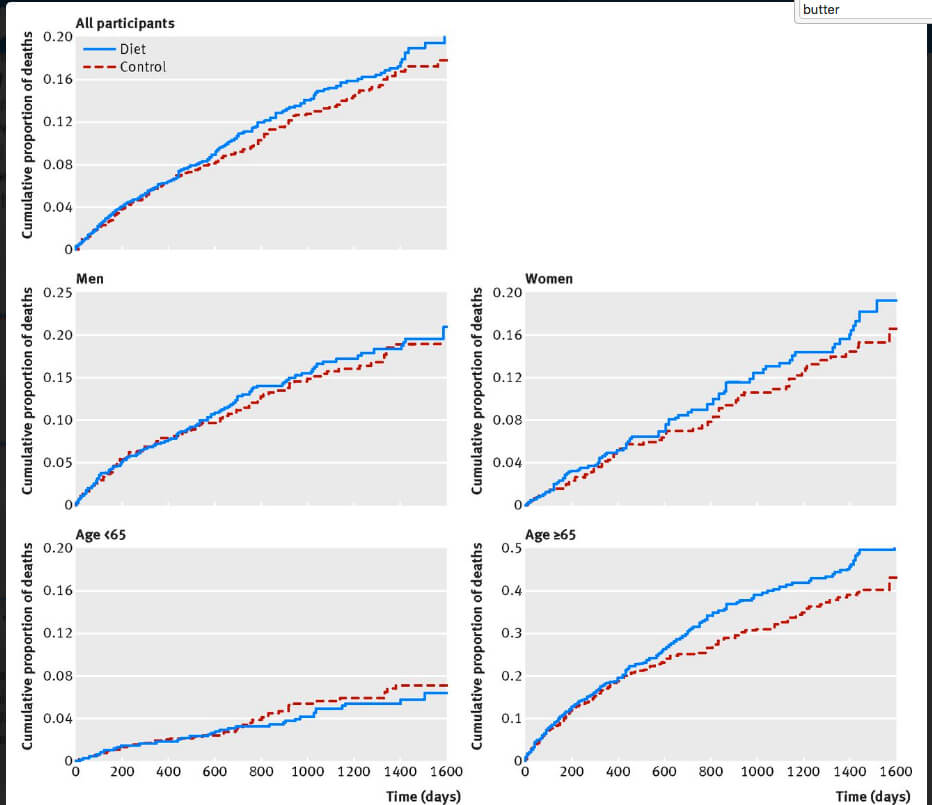
Keep in mind, the differences shown in the mortality rates of women and men and women over sixty-five are significant enough that any drug that could effectively address the effects of PUFA would be a blockbuster.
The AHA Is Giving Us Unhealthy Advice, and Harvard Doesn’t Care
Perhaps the most influential person in the nutrition world today, Dr. Walter Willet—who has a school at Harvard named after him—has called Ramsden’s study “an interesting historical footnote that has no relevance to current dietary recommendations.”
Here’s why Dr. Willet is wrong about the study’s relevance.
- The AHA ignores contradictory evidence like this at our peril. As Ramsden suggests, the AHA has been ignoring similar evidence for a long time, and “Recovery of unpublished data can alter the balance of evidence and, in some instances, can lead to a reversal of established policy or clinical practice positions.”
- The AHA still recommends “<10% of calories from saturated fats. Replace with unsaturated fat, particularly PUFA.”
- The Average American is following the AHA’s advice on fatty acids (whether they know it or not), and is now eating a diet very similar to the Minnesota Coronary Experiment’s experimental diet in terms of its fatty acid profile. Here’s my evidence:
- The MCE study diet limited saturated fat to between 8.0% to 12.3% of calories and today’s guidelines recommend limiting saturated fat to 10% of calories.
- The MCE study diet’s linoleic acid levels ranged from about 11.3% to 16.5% of calories, and today’s linoleic acid intake is probably very similar. (In 1999, this study cites linoleic acid consumption at 7% of daily calories, and that PUFA consumption has nearly doubled between then and now).
- Not only did Ramsden’s study show that the diet the AHA has most of us eating fails to reduce mortality, it actually increases mortality compared to the study’s control.
- The so-called control was radically unhealthy due its inclusion of trans fat—now accepted by the AHA to be deadly—and yet the high-PUFA diet proved either to be equally deadly or, in the case of women and seniors, notably more deadly, suggesting the AHA’s current dietary guidelines are radically unhealthy.
- Ramsden writes, “[i]t is clear from the MCE grant proposal that common margarines and shortenings (major sources of trans fat) were important components of the baseline hospital diets and the control diet (but not the intervention [high-PUFA] diet).”
- The diet the AHA has us eating may actually cause heart attacks in spite of its cholesterol-lowering effect.
- Ramsden et al point out (in the discussion section of the BMJ publication) PUFAs probably lower cholesterol because they cause “lipoprotein particle oxidation that could plausibly increase risk of coronary heart disease.”
- I’ve been warning my readers that LDL particle oxidation causes heart attacks for years, so I’m glad to see that an MD at the Lipid Peroxidation Unit of the NIH also thinks the same way. (See Chapter 7 of the 2017 Deep Nutrition entitled Good Fats and Bad.)
- The willingness of the AHA to ignore evidence that contradicts their theories on the cause of heart disease calls to question the very idea that LDL cholesterol is inherently “bad.”
Thousands of doctors across the country look at their patients’ cholesterol numbers every day and advise dietary changes and metabolism altering statin drugs based on a theory that would appear to have been proven wrong by this study. Harvard calls that an irrelevant footnote. I call it a strong indication that the American Heart Association is not looking out for your health.
Does High Cholesterol Even Matter?
It’s not often discussed, but there are decades of high-quality studies showing that death by cancer, pneumonia and other infections, and dementia are more common among folks with lower cholesterol, while high cholesterol is protective against death from these conditions.
All told, there’s enough evidence to suggest that there’s probably no such thing as ‘bad’ cholesterol. Just as having higher HDL is associated with better health, higher LDL appears also to be associated with better health as well—although that may only hold true when you’re diet is free (or nearly free) of vegetable oils. I will be offering classes on interpreting your cholesterol numbers starting in 2021, and if you are interested please subscribe to my newsletter to be notified.
To Hide the Facts About Fat the AHA and Keys Hid Smoking Data for 25 Years
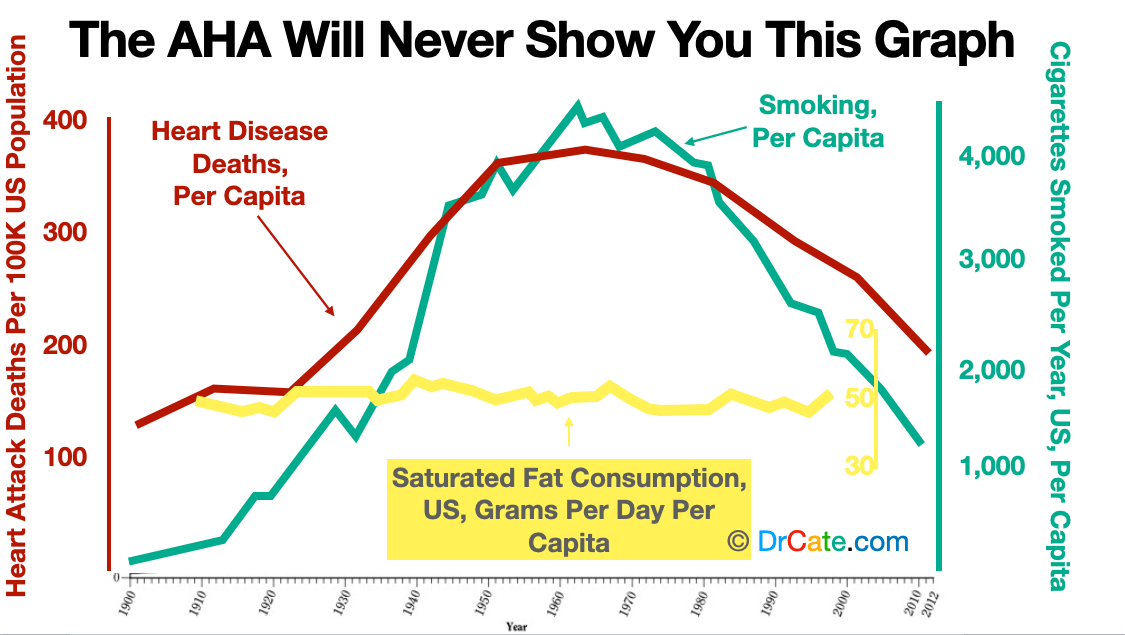
In 1956, the AHA downplayed the role of smoking, claiming, “Much greater knowledge is needed before conclusions can be drawn concerning possible relationships between tobacco smoking and increased death rates from coronary heart disease.” The AHA defends this 1956 position on smoking by stating “This is an early illustration that all research and AHA statements are based on conclusive evidence.” [sources: https://professional.heart.org/en/research-programs/aha-research-accomplishments/historic-moments-and-research-funded-by-the-american-heart-association]
To collect that evidence, they’d been planning a massive study, the organization of which began back 1953, called the Seven Countries Study.
In 1956, the same year the AHA claims that there was insufficient data linking smoking to heart attacks, they asserted, “Fat and cholesterol linked” and “assume a leading role in urging Americans to change their eating habits.” The troubling thing is that one would think taking this extraordinary measure of advising a nation to abandon the natural whole foods that had kept us healthy for centuries would require them to also definitively link either fat or cholesterol with heart disease. Seems little to ask from an institution that boasts of its insistence on “conclusive evidence.” The reality, however, was that although dietary fat and cholesterol were linked to each other, there was little to no credible evidence they were linked to heart attacks. [sources: https://professional.heart.org/en/research-programs/aha-research-accomplishments/historic-moments-and-research-funded-by-the-american-heart-association]
In 1958, the Seven Countries Study was launched. It collected data on smoking as well as eating habits, according to this statement: “When the Seven Countries Study started in 1958 the prevalence of smokers was very high and ranged from 44% in Belgrade professors in Serbia to 78% in fishermen from Ushibuka in Japan.” Available on this website: https://www.sevencountriesstudy.com/smoking-and-coronary-heart-disease/ Although the same people were simultaneously collecting data on smoking and dietary habits, making correlations and comparisons between the two quite straight-forward, the study would run for 25 years before the AHA would publish their findings on smoking, which had a much stronger correlation with heart attacks than fat intake. The only explanation is that the Seven Countries Study should be seen as the poster child of confirmation bias.
By 1961, the American Heart Association issued its first dietary guidelines that warn saturated fat raises cholesterol and causes heart disease, citing data from the same Seven Countries Study that was supposedly designed to evaluate smoking and heart disease risk. Data showing any correlation between smoking and heart disease was not ready for prime time. Had the AHA simply provided the American people the image of the left half of the graph (see above, entitled The AHA Will Never Show You This Graph), no doubt many physicians and their patients would have chosen to keep the real food and ditch the smokes.
In the same year, in his famous Time Magazine Interview, Keys actively undermines the risks of smoking, suggesting that smoking is not an important factor in causing heart disease but fat intake is. “Though Keys’s theory gained sanction from the American Heart Association last month (TIME, Dec. 26), it is still questioned by some other researchers with conflicting ideas of what causes coronary disease. The main difference is that they variously blame hypertension, stress, smoking and physical inactivity, while Keys gives these causes only minor roles.”
By 1968, a decade after it’s launch in 1958, the ten-year smoking data from the Seven Countries Study was available, according to this website which states, “The 10-year follow-up data showed that smoking was associated with a higher risk of CHD [coronary heart disease] mortality in countries where there were enough events for analysis and the strongest associations were observed in northern Europe where CHD was highest.” In other words, the evidence linking smoking and heart attacks was rock solid. But I find no evidence the AHA published this potentially life-saving information before 1980.
In 1981, deaths caused by cardiovascular diseases fell below 50 percent of deaths from all causes for the first time since 1949. The smoking rates also declined while saturated fat intake changed little.
Why Single Out Ancel Keys?
Keys apologists have told me it’s unfair to criticize the scientific integrity of anyone who isn’t alive to defend themselves. Poppycock. First of all, if any of the Ancel-Keys defenders would like to take me on, name the time and place. Secondly, there are plenty of dead people in our history who have earned our criticism and ire. What’s more, Keys’ assertions are alive and well. It is the life’s blood beating through the machinery of the American Heart Association who still benefit by citing his work. Thanks to the multiple tricks Keys used to fool the cardiologists of his day, American physicians still recommend polyunsaturated fats and are unknowingly putting their patients at risk of death and disability. This is why every doctor should learn the truth about Ancel Keys’ experiments.
Notice I’m haven’t played around with numbers. I haven’t said your HDL should be X or your LDL should by Y, although I have had such discussions becuase it can help give you insights into the current state of your metabolism. Today’s message is simple. If you’re following a low-PUFA lifestyle and the other advice in Deep Nutrition and FATBURN Fix, you don’t need to worry about cholesterol going up or increasing your chance of getting a heart attack. Get Ancel Keys and the AHA out of your head, out of your heart, and out of your diet. If you can do that, then we will have finally put Dr. Keys to rest.
- Cholesterol: What the American Heart Association is hiding from you – Part 1
- Cholesterol: What the American Heart Association is hiding from you – Part 2
- Cholesterol: What the American Heart Association is hiding from you – Part 3
- More Cholesterol articles
A 2014 article defending Keys reputation was, at the time, being publicly called to question because of how he covered up data in his famous 7-countries study. This was before the 2016 article came out implicating Keys in an entirely different cover up.
The 7-countries study controversy, covered by Authority Nutrition with a cute video.
A brief movie about Keys. At minute 22 we gain some insights into how Keys public humiliation at a scientific meeting in 1955 may have lead to his obsession with proving fat intake was the problem. Rather than being driven to find the truth, he was driven by a desire to redeem his idea, “I’ll show those guys.”
Harvard’s rebuttal of Dr. Ramsden’s study by Dr. Willet, who defends the status-quo and blames the increased deaths in the polyunsaturated arm of the study on the lack of supplemental omega-3. This suggestion seems absurd, since the polyunsaturated corn oil would have contained more omega-3 than the hydrogenated oil diet that outperformed it. He also states the study was not long enough. It was, in reality, one of the longest if not the longest study to date.
This Post Has 36 Comments
Note: Please do not share personal information with a medical question in our comment section. Comments containing this content will be deleted due to HIPAA regulations.




















And the data that he kept and used as source reference was also extraordinary poor and unreliable. 1948 was not a good year for meaningful statistical garnering.
He wrote his generation-shattering paper in 1953 because he needed something to present at a convention. If timing had obliged him to come up with something smart in the 1960s instead, he may have looked at better “studies” to form his hypothesis
I imagine that the Archeology departments of Universities world-wide are responsible for presuming paleolithic humans were massively carnivores. But one must note that the same archaic specimens examined by them reveal they had a very young life span. I think they all died in their thirties. So, can one really say, “Eat meat and live longer?”
Dr Cate,
I like your new and improved posting. If this was a court of law, your case against Keys, the AHA and their big lie would certainly be proven. Thanks to you and others for lifting the lid on the casserole dish and showing us how rotten are its contents.
The other side of the coin however, is that a lot of us have now lost much confidence in medical statistics, health care organizations, and doctors who base their diagnoses thereon.
My cardiologist now emphasizes Kato/Paleo/Fasting dieting to combat cholesterol plaquing, heart disease, and hypertension. However, he seems obliged to replace what he has surrendered on the dieting side by augmenting on the anti-cholesterol medication side. Just recently, he prescribed 4 grams of a fish oil compound per day for me. I’m wondering if he’s just sneaking in Dr Keys the eel expert back into his repertoire >: Its actually no joke as I am now suspicious of all allegedly lipid-controlling meds and am stopping them all. I’ve decided to just let nature take its course.
Udee aka Grandpaw Grizzly
Sounds like good planning on your part. Also seems like you may have what is becoming scarce in our health care system: a clinical physician who treats you as an individual not just herd member number xxxx.
HI Grandpaw Grizzly, I updated this to reflect more recent understandings I’ve gained on Keys’ relationship with the AHA, and tried to pull back on the hammering as you suggested.
I agree. Those of us in this space would be well served to pump up the volume and encouraged to freely express any moral outrage we feel. After all, we only get one life and the clock is ticking.
I’m for the Human Diet. Beans have been part of the human diet for several hundred generations and when prepared properly (soaking and optionally sprouting) are extremely nutritious. And meats have been part of a human diet for presumably far longer.
Please tell me your thoughts on Dr Gregor and how he’s opposite?
Dr. Cate, can you define macronutrient ratios for what you would consider to be a “low fat” diet? Thanks
[…] A recent example involves the hubbub about saturated fat. The data that “proved” saturated fat clogs arteries was twisted and/or fabricated from the start. The short version is that investigational studies only reported on the evidence that fit the hypothesis (see The Cholesterol Myths for a very enlightening pair of graphs) and that much of what Keys used in his own experience was implied to be butter, but was actually hydrogenated oil — a radically different substance. 1 […]
Hi Dr. Cate,
I am reading your book Deep Nutrition and really fascinated on how how you healed your knee issues with nutrition. I’m only 34 and have chrondromalcia patella and have been trying to do an anti inflammatory diet and recently added bone broth to my diet. I was wondering if your dietary recommendations would still be the same for someone who doesn’t need to lose weight? I would actually like to build some more lean muscle, but I’m actually not a big carb fan, however I am a protein eater. I was just wondering if your guidelines would be the same, I’m not super active anymore with the knee issues but still workout praying healing will come. Thank you for your time.
For building muscle it’s helpful to get 2-3 meals per day with 20-30gm+ high quality (real food, animal) protein. The lysine content seems to stimulate muscle protein synthesis.
Dr. Cate,
Are you familiar with Dr. Greger? He has a completely opposite opinion in regards to nutrition.
nutritionfacts.org
Dr. Greger, nutritionfacts.org, is the best (if not only) source of objective, scientifically-based, information that is non-profit and totally free of commercial interests. His brief research-based nutrition videos are a wealth of information (quite entertaining) and available at no cost.
Brad that’s not entirely true. Dr Gregor is not totally free of commercial interests. His income, his employer, is the humane society and although they do great work for animals, when it comes to human health, they do have a powerful pro-vegan agenda. Check it out.
I’m sorting thought the sources.. It seems Dr. Greger is totally against animal based products, meat, butter and such. and I found your site and Mark Sisson’s is contrary to his views, pro-anumal products. Dr. Greger is way pro- bean diet and Mark is against it (not sure your position, thought)
It seems like two different and opposite camps.
Hi Cate,
Not sure if you will get to read this but I would love your help. I recently listened to you interview with Dave Asprey. Loved all of your knowledge on veg oils. I am currently compiling my notes for my own podcast on veg oils, and was wondering if you had any links to scientific studies on two aspects you mentioned. One being that veg oils damage epithial cells, and one that they gobble up anti-oxidants. I’d love to cite some studies in my notes.
Many thanks
Karen
HI Karen,
Dave and I discussed that vegetable oils interfere with something called endothelial function, which is how your body regulates blood flow. So we weren’t talking about epithelial damage. I explain why endothelial function affects your ability to concentrate, among other things, and discuss the antioxidant issue in Chapters 7 and 8 of Deep Nutrition and include citations to support all claims.
HI Karen, Dave and I were referring to “endothelial function” and the study I mentioned is here http://www.sciencedirect.com/science/article/pii/S0735109798006810 Many more in Ch 7 of Deep Nutrition!
And when all is said and done, history will remember Ancel Keys as a groundbreaking scientist. As for you, you’ll be remembered as the quack whose diet advice caused the Lakers’ rankings to drop faster than panties on a porn set.
You really should look at these videos. You might learn something.
http://plantpositive.square…
I’m sorry, but Keys’ didn’t cover up anything in the sever countries study. It was a multi-country, multi-cultural epidemiological longitudinal study spanning many years and involving many international institutions. What you’re talking about is his paper from 1953, where he plotted 6 counties fat consumption against heart disease. He was accused of leaving out 16 countries data in that paper, but he gave good reason; the data was poor and unreliable.
Oops I’ve mixed up the different tactics Keys’ used to prove his point in the 6 versus the 7 countries studies. Thanks for pointing that out. In the 6-countries study he excluded entire countries when the data didn’t match what he wanted to prove. In the 7-countries study, he used entirely more complicated statistical cheats, delineated by both Gary Taubes and Nina Planck in their books. I’m a fan of trying to be fair, but Key’s made it clear that he had an agenda and was financially backed by the sugar industry. Plus, he didn’t even practice what he preached as far as not eating red meat because somewhere along the way he wrote or was quoted as saying that he and his only ate brisket (or some specific cut) for breakfast 3 times a week….I think it was in his book on the Mediterranean diet that I read that….Not sure anymore as it was over a decade ago.
Good article. The recently published revision of the Sydney Diet Heart Study, also by Ramsden, reported similar findings which were also ignored in the initial article. These are major revelations and should be sending a shock wave through the nutritional science establishment. It is fascinating how they are so wedded to their dogma that they cannot conceive that it is wrong even when the very foundations are clearly shown to be the reverse. Another great folly of medicine like Semmelweis, bloodletting, etc. How many more will be harmed before we right the ship?
Dr. Cate, could you develop graphs showing the increase in heart attacks and strokes over time in relationship to the change in consumption of fats? The relationship wouldn’t be immediate but there should be a delayed one.
A graph like that should then be persuasive to other doctors.
Thanks for developing this article!
Interesting idea. It would be heavily confounded by smoking rates, which also paralleled a lot of this stuff. See my graph posted in response to Kurt Lass, the day prior. What do you think?
Very well presented. Over the past couple of years I significantly increased my dietary fat intake, especially saturated fat, while dramatically restricting refined carbohydrate intake. The result? Effortless 25 pound weight loss, 3 inch waistline decrease, reduced cravings, and improved mood/energy level. I write about this at https://www.yourorthomd.com/orthopedic-dietnutrition/why-would-an-orthopedic-surgeon-care-about-diet
While Keys was certainly responsible for the original development of the K Ration, he is unlikely to be responsible for the cigarettes. Tobacco and cigarettes were included in US military field rations long before the K Ration was developed…
Good point. Still, I give him thumbs down for expanding the trend. Smoking rates ballooned after WW2. https://uploads.disquscdn.com/images/7780b5f7811976026b37e89bbdb1648857cbd63e91d99606f1890befbf133613.gif
Pure association only… Tobacco use in the military had a long history prior to WW2 – Quite a lot of evidence for this – See: https://smokingjacketmagazine.com/2014/11/11/smokes-for-the-boys-a-history-of-smoking-and-the-military/ for a start. Smoking in the military was promoted via culture, patriotism, tobacco industry and governments. Cigarettes were also included in WW2 “C Rations” which had nothing to do with Keys. Keys has a lot to answer for, but it is important to be accurate about what he actually did.
I want to hear from you! Do you agree with the arguments here? Any ideas about how we get more doctors, dietitians and other who are in the ‘system’ (by which I mean they accept health insurance) on board?
I have been following the literature in this field for over 4 years, ever since reading Gary Taubes’ epic volume Good Calories Bad Calories. It has been and still is great experience.
I totally agree with what you presented, and I admire your leadership in this regard, because it is clear that many in the health profession do not want to publicly dissent with the conventional wisdom. As we all know, there are strong political and Industry forces at work to discredit dissenters and make their life difficult. Just look at Dr. Noakes, Dr. Fettke, and also several other doctors or dieticians. Just the fact that the American Dietetics Association clearly states that any dissent from what the association guidelines state by a member is punishable by exclusion from the association. That is a serious deterrent, and should not be supported by law. So we can see that the establishment is fighting back, as big money is at stake, as well as scientific reputations. The only way I see the situation turning around is through medical leaders such as you who stand up for what is right and push ahead in spite of all the politically supported road blocks. The internet make is all possible, and I am very grateful for that. Please keep your good work.
Hi Cate,
While I welcome any blog pointing out that real foods, like butter and eggs, are healthy and omega-6 vegetable oils are not, as you’ve said “I want to hear from you! Do you agree with the arguments here?” there are some points that could do with clarification…
1) Keys was sometimes erratic in his fat terminology (describing cakes and ice cream as “saturated fats” as late as 1970 in The Seven Countries Study) but he knew what he was doing in terms of experiments.
There is indeed a paper called “Hydrogenated fats in the diet and lipids in the serum of man”, but it is about hydrogenated fats! The paper describes experiments involving 23-27 men where safflower oil was compared with hydrogenated safflower oil and corn oil was compared with hydrogenated corn oil. (For interest, consumption of the hydrogenated vegetable oils resulted in higher total cholesterol than the non-hydrogenated versions). Examination of this paper, or others of Keys at the time, show his lipid knowledge (dietary and serum) to be impressive.
Another paper, from four years earlier (1957) “The effects of different food fats on serum cholesterol concentration in man”, with the same author team, administered butter, olive oil, corn oil, coconut oil, sunflower seed oil, sardine oil and cottonseed oil in separate tests to see what impact these had on serum cholesterol levels. For each fat, Keys, Anderson and Grande documented the saturated, monounsaturated and polyunsaturated content – something not enough people are aware of today.
The main finding, which Keys presented against saturated fat, was in the summary volume of the Seven Countries Study. Here he claimed: “The average serum cholesterol values of the cohorts tended to be directly related to the average proportion of calories provided by saturated fats in the diet” and “The CHD incidence rates of the cohorts are just as closely related to the dietary saturated fatty acids as to the serum cholesterol level.” Not terribly assertive on either point.
In this same study, Keys reported “Serum cholesterol averages and CHD incidence rates were not found to be related to the percentage of calories provided by polyunsaturated fatty acids in the diet” (this quotation continued: “and were only slightly related to total fat calories.”) This was when Keys changed his view that total fat was a factor in heart disease. This is not widely enough known.
I’m not aware of any claim made by Keys that eating PUFAs would help people live longer.
2) The Ramsden re-evaluation of the Minnesota Coronary Survey (MCS) was a brilliant piece of work, but I’m not sure it was necessary. The MCS started in 1968, but the main paper was published in 1989 (“Test of effect of lipid lowering by diet on cardiovascular risk. The Minnesota Coronary Survey”). Why did it take so long? You rightly praise Gary Taubes for his work in this area. In Good Calories Bad Calories, GT reports “When I asked Frantz in late 2003 why the study went unpublished for sixteen years, he said, ‘We were just disappointed in the way it came out.'”
The 1989 MCS publication concluded: “For the entire study population, no differences between the treatment and control groups were observed for cardiovascular events, cardiovascular deaths, or total mortality.”
This study simply didn’t support the lipid hypothesis. Plus, I’m not sure it’s fair to attribute this study to Keys. There were seven authors on the 1989 paper and Keys wasn’t one of them. Frantz may have been in Keys’ department and I’m aware that Ramsden refers to Keys as “co-principal investigator” (based on the research grant application?), but I’m not convinced that this can be pinned on Keys.
3) Here’s how vegetable oils (plant sterols to be specific) can lower cholesterol by the way – while being associated with increased risk for CHD (http://thescipub.com/abstract/10.3844/ojbsci.2014.167.169)
4) It is common, but wrong, for people to mix up the 1953 Keys Mount Sinai presentation – where data for 6 countries were presented while data for 22 countries were available – with the 1970 Seven Countries Study, which was always about 7 countries (16 cohorts). Tom Naughton is right in his video (he doesn’t mention the source of the graph); Authority Nutrition is wrong and so is your link across.
I think that Keys does have a lot to answer for and I’ve criticised him myself a number of times. However, we’re taking on conventional ‘wisdom’ when we write blogs like this, so we need to be accurate as well as challenging.
Best wishes – Zoe
Thank you for your thoughtful writing. Your statements are valuable. These concepts are complex and easy to misread so thanks for pointing out what I could clarify.
1) My point was not that Keys lied about his use of hydrogenated fats, but rather that used our ignorance against us. When it came to speaking about the results of his studies to reporters he never explains what hydrogenated fats are, and typically brought up butter and animal fats as if to imply that’s what he studied. As I hoped the cartoon of the mouse and the cat would clarify, doctors didn’t know what the heck hydrogenated fats were, but they did know what butter was. So it was easy to confuse us.
2) The Ramsden study was invaluable because he published never before published results of the autopsies. In addition, it helps to again highlight, as I did here, that the “control” diet was loaded with trans fat and the PUFA diet performed worse than that, which I think it a key detail we needed to know. And no doubt Keys didn’t want his name on a disappointing study, eh?
4), I am not mixing up Keys’ studies. My point, and quite possibly Naughton’s is well, is that his 7-countries study was done on those countries that he knew ahead of time (because he’d done the 22/6 countries study by that point, along with other surveys) would ultimately support his data.
Dr Cate,
I recently read Ramsden’s work. From it I draw the perspective that his data was more in line with modern statistical science and he points out Keys only proved (with erratic data) a co-relation between dietary fats and serum cholesterol. A co-relation is not necessarily a function-thereof i.e. not all permanently resident cholesterol comes only from dietary fats. And the relationship of cholesterol to CVD deaths was not at all proven; thus earning only a dotted line from Ramsden, not a cause-and-effect straight line.
Just recently, I experienced an accidental experiment with interesting results. I had blood drawn in May17 for a basic metabolism review but the lab did a lipids report as well. The blood was drawn about 30 minutes after I consumed a full saturated fat and cholesterol breakfast (bacon and eggs) because I did not know they were going to analyze lipids too, which in the past always required fasting. So Zero fasting this time and the lipids showed my total chol and triglyceride numbers through the roof! This was upsetting, so eight weeks later, in Jul17, I went back to the same lab for another lipids test after 13 hours fasting. This report reflected my total chol and trigs about 500% lower and at the low end of the acceptable scale.
So, at least for my body, maybe dietary fat and cholesterol does cause a spike in serum numbers, but it is not the kind that sticks around to turn into plaque, which is after all what heart disease is. Its not the fat and cholesterol that will give me a heart attack, its if that stuff sticks to the inside of my arteries and blocks the blood flow. I wonder which one of my cardiac pills helps with that…
Hi Dr Cate. Books like yours and having a platform where you go grassroots to ppl is the key and a good start.
When patients become informed and have the information needed to take control of their own health, then we can talk to our physicians and become our own guinea pigs to prove that deep nutrition works.
I believe drs don’t change bc they havent seen real results in front of them.
I have T2 diabetes. I refused metformin and the other drugs until i can first fix myself with nutrition and excercise. When I do, I want my next blood test to be DRAMATIC in the changes so that I can prove it to my Dr.
I intend to keep a detailed food journal and glucometer results so she can see the plan and its effects.
If enough patients do this we can slowly but surely compel more Drs to at least learn about nutritional interventions first or in adjunct with Rx.
Thanks for writing Deep Nutrition. Its such an excellent piece of writing. Its actually one of the best books I’ve read in general, not merely out of other nutrition books.
I will fill you in on the results, when I return in 3 months to see how my blood test results turn out. Perhaps I will be Diabetes free!
Thanks!
Dear Dr Cate,
I think you may need to more precisely define the bandwagon and where it is heading, before you can “get more doctors, etc, on board.” I have read all the arguments but I am unclear as to which one won…Some kind of synthesis of well-based conclusions seems warranted. The anti-fat-of-any-kind Mediterraneans are strongly entrenched in my health care complex and require something almost biblical in rhetoric to even budge them.
As to Dr Keys’ “study,” I seriously question the validity of the source data that he looked at. It seems the information was originally collected in 1948. At least two of the countries surveyed, Japan and Italy were barely three years out of an utterly devastating war. I question the accuracy of bureaucratic statistical systems under those conditions. I wonder if the other four nations were in any better shape at record-keeping, just because they won the war. British institutions certainly suffered a lot of war damage also.
In summary, I think Dr Keys’ data was most likely defective at the root level. If he was a graduate student today presenting a thesis based on such questionable data, and I was his mentor, I would send him back home to start over again.
On the point of ethics, whether or not he maliciously manipulated the available information to make an academic splash seems no longer important, any more than the fact that I had to needlessly sacrifice my passion for bacon and egg breakfasts for the last 30-some years! As an avid carnivore, I am all for the more-meat-less-berries new slant nutritionists seem to be favoring. Perhaps what we need is less hammering at past mistakes and more and better proof in support of new concepts for healthier bodies.