The cause of gluten intolerance is not gluten. It's immune system dysfunction. Learn why your immune system starts to go off track, and what you can do to right your immune system's wrongs.
What is celiac disease? A recipe for recovery beyond gluten free.
Table of Contents
- Celiac disease is a set of symptoms associated with gluten intolerance.
- Why is gluten intolerance suddenly so common?
- I think the answer is inflammation, and the resulting genetic change.
- Real Reason for Hope: Epigenetics and Gene “Intelligence”
- Why some people make antibodies to gluten: Immune system confusion
- How Molecular Mimicry Causes Celiac Disease
- To cure celiac symptoms, auto-antibody levels must drop and you must develop “tolerance”
Celiac disease is a set of symptoms associated with gluten intolerance.
Celiac disease develops when a person makes antibodies against a wheat protein called gluten such that eating anything containing gluten results in intestinal discomfort and a variety other symptoms including joint pain, skin rashes, and fatigue. Gluten is also present in barley, oats, triticale, and a few other seeds, and is often added to baked goods as a separate ingredient.
Why is gluten intolerance suddenly so common?
You could say gluten is the new cholesterol, in that gluten is being identified as the cause all kinds of illnesses and it has been suggested that nobody should ever eat it anything containing traces of it. But as is the case with cholesterol, pinpointing this single food component as the new universal-scapegoat is misguided. The way I see it, celiac disease is part of a larger epidemic of allergic disorders that include all food allergies, allergic rhinitis, and asthma—all of which are in the midst of a dramatic rise.
This article is continued below...(scroll down)
Whenever something new like this comes over the horizon, I like to always take a step back and examine the larger picture. When I do, I see the new explosion in rates of gluten-intolerance not so much as the result of anything inherently unhealthy about gluten, but rather as a sign that the processing that renders gluten harmful has lead to widespread immune system confusion. So in that sense, gluten is the canary in the coalmine, warning us of a potential impending explosion in the rates of intolerances to all kinds of processed foods.
When I started out in medicine in the 1990s, the most common food allergies were soy, eggs, peanuts, tree nuts, shellfish, and dairy. Each was far less common then than now. Wheat wasn’t even on the list. While I lived in Hawaii, by some measures the healthiest state in the nation, food allergies were almost non existent among my older patients. As the years went on, I noticed more and more kids coming in with food allergies. Then I moved back to the mainland where the number of young adults and children with foods allergies of all kinds blew me away.
My own experiences are echoed by doctors all over the country and reflected in national statistics which show that rates of food allergies have risen dramatically over the last decade, especially among the younger generations.
Gluten-free recipes are suddenly all the rage
The epidemic has taken the entire medical community by surprise and so far even our top academic practitioners have no good explanation for the recent spread of celiac disease—or the other food allergies. And so, most of my patients have had to educate themselves. They come to me after reading theories on the cause of gluten intolerance propose by a collection of health and wellness personalities.
Here’s a synopsis of the top theories circulating around the net, and my critiques:
- Wheat has been bred for high yield, rendering it unsafe to eat.
(All crops have been bred for high yield, and wheat is no exception.)
- Man evolved as a hunter-gatherer, and should not eat wheat because it is an agricultural product.
(Ditto: All crops are agricultural products, and wheat is no exception.)
- Wheat is a grass, and we haven’t had enough time to genetically adopt to eating grasses.
(Rice is a grass and it doesn’t cause celiac.)
- Wheat is a seed, and all seeds contain antinutrients. In the past, people used to sprout and soak seeds to increase their nutrient bioavailability, so we should too.
(While I’m all for increasing nutrient bioavailability, this theory, like the others, still fails to explain why gluten —a protein, and not an antinutrient—causes sickness.)
So far, I have yet to see anyone discuss gluten intolerance in the context of this epidemic of food allergies and allergic disorders. As I said, ALL allergic conditions, from asthma to eosinophilic esophagitis to rhinitis and eczema, are increasing, and not just in the US, or developed nations. We’re experiencing a worldwide epidemic of allergic diseases of all kinds. Why?
I think the answer is inflammation, and the resulting genetic change.
As I explain over several chapters in Deep Nutrition, the consumption of free-radical-causing vegetable oils combined with excess protein glycation from excessive sugar ingestion create a toxic environment for our bodily functions. None of our body’s systems can function normally in this toxic environment, not our hormonal system (which affects reproduction and genes), not our skeletal system, not our nervous system, and not—here’s what inflammation has to do with celiac disease—our immune systems.
The development of celiac disease is an important sign that your diet may be interfering with the normal function of your immune system. I like to help my patents understand that gluten intolerance is not, as we commonly hear, a strictly genetic disease, and supporting this idea is the fact that most people with celiac also have one or more other allergic disorders. Immune dysfunction can have even more serious consequences than celiac, including cancer and neurologic degeneration, and I discuss this below where I talk about molecular mimicry.
Inflammation also interferes directly with gene function and can cause abnormal or imperfect DNA replication, which is another fact that gets overlooked in most discussions of gluten intolerance. Through no fault of their own, women have been following dangerously pro-inflammatory diets during their pregnancies because our culture promotes wrong-headed dietary advice, and these pro-inflammatory foods are cheap and readily available.
Because of these nearly ubiquitous toxic exposures, however, over the past decades many babies have been born with genes scarred from exposure to inflammatory chemicals during key periods of replication. Today, the younger generations suffer from never-before-seen and sometimes disabling sicknesses because they have very fragile overall systems that will readily malfunction on anything other than a perfect diet.
And few parents are aware of, not to mention ready to provide, that perfect diet.
Real Reason for Hope: Epigenetics and Gene “Intelligence”
Fortunately, however, damaged and malfunctioning genetic material has the potential to regain normal function. This has to do with the fact that most of the genetic damage is confined to the gene regulation system, and does not affect the DNA itself. So if we provide our bodies with a rich variety of healthy foods and keep inflammatory exposures to a minimum, metabolic processes that currently malfunction may be able to repair themselves and begin to function normally again.
Why some people make antibodies to gluten: Immune system confusion
A two-step process triggered your body to make antibodies against gluten.
First, you ate processed foods that contained a distorted form of gluten that alerted your immune system to the presence of gluten. This immune-attraction is called an adjuvant effect. Gluten develops its adjuvant properties during processing when the protein reacts with sugar and distorts into all sorts of configurations, generating compounds that did not exist before processing.
Second, you also ate foods that promote intestinal inflammation. Adjuvant plus inflammation usually means you have an infection, and when you have an infection, your white blood cells manufacture antibodies to attack the invading organism. So your confused immune system mistook gluten for an invader, and you started making antibodies against gluten. Though processed and distorted, gluten, as with the windmills Don Quixote perceived as ferocious giants, does not pose an infectious threat, and the immune attacks are a tragically useless pursuit.
The foods containing proteins most likely to attract the attention of your intestinal immune system, like windmills dotting Don Quixote’s landscape, are those that meet two criteria:
- They contain complex protein molecules and an abundance of sugar molecules
- They are consumed often in processed form.
The most common allergens, wheat, soy, and casein meet both criteria. Eggs, another common food allergen, are included in vaccines and may trigger an antibody responses in some people for that reason.
The foods that promote intestinal inflammation and trick your immune system into thinking there’s a bad bacteria on the loose and launching it’s tragically useless and painful attack also meet two criteria:
- They promote free radical formation, which makes your immune system think you are infected with a pathogenic bacteria.
- They are high in starch, which gets rapidly fermented into sugar and invites overgrowth of bacteria that are borderline pathogenic, like yeast, which further confuses your immune system.
Statistically speaking, if you have one food intolerance, you’re more likely than the average person to have another. For instance, many people with celiac also have problems from dairy because the same sequence of events that played out with gluten also played out with a milk protein called casein, which, like gluten, is added to lots of processed foods. The same applies to soy, if you have soy allergies, eggs, if you have egg allergies, and so on.

So far, I’ve described only the reasons you have antibodies against gluten. People who suffer from celiac also have joint pains and skin rashes because the antibodies against gluten also just so happen to cross react with these tissues. The process is called Molecular mimicry.
From antibodies in the gut to problems in the skin, joints, and nervous system.
I do not believe, as some have proposed, that most people’s joint and skin symptoms are caused by particles of food traveling undigested to reach these tissues where they lodge and promote inflammation. I believe what happens is antibodies against food happen to be shaped so that they also bind to bodily tissues, launching a painful or disabling immune attack against your joints, your digestive system, or even your nervous system. This is the hypothesis proposed by scientists who study Molecular Mimicry.
How Molecular Mimicry Causes Celiac Disease
When molecules of different origin have segments in common, our immune cells may confuse one for the other. This is the accepted explanation for auto-immune diseases like lupus in which the troublesome agents are “auto-antibodies”—antibodies that attack you, rather than invading pathogens. The auto-antibodies bind to your own tissues where they attract white blood cells that can launch an attack. The effects of such an attack against your own body can cause, for instance, the symptoms of Lupus, an “auto-immune” disease.
Why antibodies sometimes attack their host (you).
Unlike cells, which are driven by the intelligence in their DNA, antibodies are mindless. They are large, Y-shaped proteins studded with sugar that the body manufactures after an infection to prevent you from getting sick from the same infection twice. Once you make antibodies to a pathogen, the next time the same organism tries to take root in your body the antibodies recognize it’s molecular fingerprint and bind to it, drawing a white blood cell attack that eliminates the invaders before you even feel sick. This is how it’s supposed to work.
Antibodies recognize bacteria by “feel” the way you feel around for keys in your purse.
Antibodies seek invading bacteria by “feeling” for matching patterns of protein and sugar (the molecular fingerprint) as they circulate through the blood and through the spaces between your cells. When the antibodies identify a fit, they slip around the matching molecular fingerprint like a glove around a hand, and then snap on tight. Once snapped on, patrolling white blood recognize the snapped-on antibody as a signal of trouble, and release chemicals that call for more white blood cells to rush in and destroy the invader.
The antibody-making system is not absolutely perfect. Sometimes your body will make antibodies that happen to match the molecular fingerprint of one or more of your own tissues (molecular mimicry). Fortunately, your body has several checks and balances in place that are designed to result in the destruction of these “auto-antibodies.” This process of destroying antibodies is called “tolerance.”
But those checks and balances fail when your immune system is not functioning normally, for example under times of extreme stress, sleep deprivation—or when eating a pro-inflammatory diet. Under these difficult conditions, your immune system is less likely to properly complete all of its checks and balances, “tolerance” never develops, and the auto-antibodies can end up misleading your white blood cells into launching an attack against your own tissues.
The exact tissue affected depends on the exact shape of the antibody. Celiac sufferers often make an antibody to a protein called tissue transglutaminase, which is located in the joints and skin, as well as the GI tract. Another common antibody is called “anti-gliadin” and this antibody is thought to be responsible for nervous system inflammation and neurologic disability associated with celiac. But there are probably many other antibodies associated with celiac disease that scientists have yet to identify and so we can not yet test for any of them.
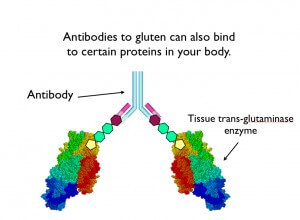
To cure celiac symptoms, auto-antibody levels must drop and you must develop “tolerance”
The results you get from cutting gluten from your diet depend on how far your antibody levels drop. The reason some celiac patients feel better after stopping gluten is that the antibody levels have already dropped. The reason others don’t is that the antibody levels have not dropped.
To get auto-antibody levels to drop faster, farther, and potentially even permanently, you have to eliminate not just gluten, but all foods that cause inflammation. And again, the most common are vegetable oils that promote random free radical formation, and carbohydrate-rich foods that promote random tissue glycation.
While the idea that a person with celiac may someday even be able to eat gluten again is so-far untested, I have reason to believe it is at least theoretically possible.
We know that, thanks to the built-in “intelligence” of the immune system, auto-antibodies can be recognized as unnecessary and deleted. So a person who once used to make, for instance, IgA antibodies to tissue-transglutaminase, no longer makes these antibodies and auto-immune attacks stop for good. Though this presents reason for hope, I have to say that at this point I would not recommend anyone diagnosed with celiac by antibody testing or who has definite joint pains or rashes after eating gluten take the risk of re-exposing themselves.
A Healthy Diet To Recover From Celiac: Three Steps
As I’ve said, avoiding gluten is an essential step in recovering from celiac, but it is not enough. You also need to avoid factors that caused the faulty antibody production associated with celiac (and other food allergies) in the first place. The first two-steps for making a full recovery from celiac are:
Step One: Avoid vegetable oils, and keep your total carb consumption under 100 gm per day.
Step Two: Retreat to ‘safe” starches
The antibodies that cause gluten intolerance and celiac were made by mistake and you must eliminate them to eliminate symptoms of celiac. Avoiding gluten is an essential step. Many gluten free recipes make use of so-called “safe starches” (a term first coined by the authors of The Perfect Health Diet).
I define safe starches differently for celiac sufferers, or anyone with persistent digestive difficulties that could represent celiac, than I do for people without these health challenges. Safe starches for the general population are high-carb foods with one or more of the following traits:
- They contain a relative abundance of anti-oxidants (i.e. carrots or beets)
- They are low in protein (ie potatoes, rice)
- They are not commonly used in infant formulas or other processed foods.
Even if you do not have celiac, these kinds of starches will still be better for you. For celiac sufferers, or anyone with persistent digestive difficulties that might represent celiac, I add the fourth trait:
- They are gluten free.
Step Three: Promote healing.
For optimal recovery, I advise my patients to eat superfoods that promote rapid digestive recovery into their diet. Two of the four pillars of world cuisine defined in Deep Nutrition promote optimal digestive health, and these are collagen-rich bone broths and probiotic-containing live-cultured, fermented foods like yogurt, kimchee, real pickles, and sauerkraut.
Anna Voccino is a radio personality with celiac who is also a talented home cook with several recipe books that give you fast, easy gluten-free meals. Her website: https://annavocino.com/eat-happy/
Sean Croxton at Underground Wellness: Sean invites speakers to discuss all sorts of under discussed health topics and his videos, podcasts, and posts are loaded with personality.
Please note: Please do not share personal medical information in a comment on our posts. It will be deleted due to HIPAA regulations.
This Post Has 45 Comments
Comments are closed.
Note: Please do not share personal information with a medical question in our comment section. Comments containing this content will be deleted due to HIPAA regulations.

















Thank you, thank you, thank you for all your work. For 5 years I jumped from one specialist to another. I have been diagnosed with RA, Lyme disease, depression, anxiety, hormonal imbalances (that led to a full hysterectomy and oopherectomy) degenerative disc disease (that lead to ACDF at C5/6), and myofacial pain syndrome. I had neurological symptoms that led doctors to test me for MS and lupus. Never did I have noticeable digestive system issues for doctors to suspect a gluten allergy. Guess what! I solved the problem myself. I was trying to loose weight quick for a wedding so I jumped on keto for 2 months. Three weeks into the diet I felt 99% better. I started to add back carbs starting with starchy veggies and fruit with no issues. I left gluten last. All it took was one meal and my myofacial pain and nerve pain was back. That’s it. I was done. It’s been a year and I never look back. I eat 100% gluten free now. Mostly whole real foods. Rarely do I even eat processed gluten free foods. When I finally approached my primary 6 months later she said at this point I had been gluten free for too long to get a positive celiac test. But she is 100% with me that gluten caused my inflammation. Even some gluten free foods like oatmeal will cause a reaction if I eat a bowl more than once a week. Your article and your research show the science of what my body does. I cannot thank you enough.
[…] Read about why your immune system malfunctions and how celiac causes joint pains on this post. […]
[…] Read about why your immune system malfunctions and how celiac causes joint pains on this post. […]
Greetings Dr. Shanahan,
In your youtube video, at the 5 minute mark, it states, “cutting carbohydrate intake down to 100gm/day or less.” Are you advising Celiacs sufferers, who have given up all gluten, to reduce ALL sugar intake to less than 100gm/day OR each type of sugar, as listed in the video, to less than 100gm/day?
In addition, can you post any of the information from the book you are working on “which will provide a program for adapting an anti-inflammatory optimal diet of traditional foods that are delicious, fast, and affordable”?
1. Total intake.
2. You ought to look into reading the books we’ve written. You’d have known the answer to #1 🙂
@John: Hi, I also have Celiacs Disease and was diagnosed during Aug 2008. On your comment: ”poor bone density” and ”muscle joint pain”: it sounds as if you could have deficiencies. I would suggest that you see your specialist (a Celiac should go for yearly check ups) and get some blood tests done for deficiencies. Poor bone density – Calcium, Vit D, etc. Muscle/joint pains – Vit B12, etc. But you also have to check out your iron, very important. Don’t take a supplement for iron if you don’t know your iron status-dangerous. If you had very bad damage to your small intestines you might experience absorbtion issues. It could take long (even years) before the villi heal, if that is the case. Calsium supplements should be gluten free ! Make sure that it is a good product that absorbs right (not in your bloodstream, but to the bones !) Calsium should be taken 2hours after your last meal/drink and you should wait 2hours before you eat or drink again for good absorbtion. Also the supplement should have the right ingredients to not only help absorbtion but also absorbtion to the right places in your body. Discuss this with your pharmacist. Use enough water to help the calcium disolved. I use it just before I go to bed. Your store rooms for calcium could most likely also be empty. Don’t skip the supplement until your body could skip one day without a calcium supplement easily without pain. Don’t use other medication or supplements with calcium, use it on it’s own. (Remember that the right calcium supplement already have other supplements that is necessary in it.) Vit B12 helped me with the pins and needles and pains in my legs, arms, hands, back, etc. Another important thing is that iron and calsium compete for absorbtion to your bodies storerooms. If you are already using an iron supplement or if you are going to use an iron supplement in future, make sure that you use a form that will absorp easily, but will not be in conflict with the calcium supplement that are using. Please discuss this with a senior pharmacist. Important to know is that I am using a gluten free probiflora to help me with absorption of foods, etc. All the beforementioned made a huge difference in my daily life regarding pain & energy. Hope this will be of some help to you ! GlutenFreeSA Greetings. Teresa
I was diagnosed with Celiac almost 3 years ago. I have poor bone density, especially in my right hip, where I have alot of muscle/joint pain that I go to physical therapy for. My lipid profile is very bad because my LDL are the small particles and at very high levels.
I started low carb’ing again and I finally fought my way down from my highest weight of 216 down to 198 ( I used to be 74 inches tall and now I am 73.5), but my lipid profile hardly budges and the doctors want me to take statin drugs. At 51, I am nervous that all this inflammation has led to clogged arteries. I have exercised all my life so I am hoping that it helped me. In addition to osteopenia I also have low T but my TSH appears to be in the normal range (2.5)
So do I go completely vegan as Essylstine says, or do I go paleo? I am afraid to eat not only grains now, but also am afraid of eggs, dairy, and meat because of my cholesterol numbers. I honestly don’t even know what 100 grams of carbs equates to in a food source. can you try to unravel my dilemma?
An example, 1/3 cup cooked pasta, 1/2 a banana, 1 slice bread, and 3 prunes all have 15 gm carb. Lots of resources online for you!
Dr. Cate,
Today I finished Deep Nutrition and I have a few questions. We have been gluten free for about 2 years. Some of our issues have cleared up and some not so much. In short, what if one (me and mine) has been “doing” a mostly Deep Nutrition,(prior to reading), lifestyle for 5-6 years and are still dealing with inflammatory issues, weight gain, adult acne and pre-pubescent blackheads/pimples, 2 of us with an autoimmune disease, 3 with arthritis, 1 with high blood pressure and so on.
I will give you a glimpse of our lifestyle. I milk my own Jersey, eat my own eggs and meat beef, chicken goat; grow many of my own veggies year round, eat lots of cream and butter, the fat on my meat, bone broth; within the last year have given up vegetable oils except olive; gluten free for 2 years; very little organic cane sugar say less than 2-3 T. daily, many days none ; wine and cheese of my own making, mostly my own and daily; milk and/or water kefir daily; work at home is my exercise along with stretching; 90% organix in everything. I am sure we don’t get enough aerobic exercise, but plenty of day to day chores on a family farm.
So, where are we (me, since I am the chief cook and bottlewasher) going wrong? Too many “complex’ carbs ie brown rice pasta or homemade GF bread? not enough greens? too much fruit? too much wine? just too much?
Any thoughts and help would be welcome. Please gently correct me if this not for this group/forum and redirect.
All of your suggestions (Too many “complex’ carbs ie brown rice pasta or homemade GF bread? not enough greens? too much fruit? too much wine? just too much?) are excellent points for consideration. In fact, they are questions I would ask if you came to my clinic. I bet you are now are on your way to sorting it out on your own but if you need help there are more and more listings every day for practitioners who can help. You will find the links with google searches “paleo physicians network robb wolf” or “low carb physician jimmy moore” or “physicians for ancestral health” and of course you are welcome to schedule a consultation.
Is olive oil inflammatory? And what about butter?
Thank you Dr. Cate, This is really helpful.
Dr. Cate,
My 22 month old daughter had an allergic reaction to peanut butter at the age of 13 months (itchy rash on neck and mouth). I had her tested for allergies, and the results showed allergies to peanuts, walnuts, sesame and almonds. We were told to avoid peanuts but not the other nuts UNLESS she showed a reaction, which she later did with walnuts. At the time she ate almond butter regularly but never showed a reaction. I’m confused as to why it is recommended to avoid one allergen and not the others, only based on a visible reaction. As for her diet, we generally eat “Paleo”, with occasional indulgences of gluten. She was never on rice or wheat cereal as an infant. We do eat dairy, mainly yogurt. The allergy MD recommended that we come back in a year for more testing, and he hopes that she will grow out of the allergy. My question is, what is the best advice for how to feed her to give her body the best chance of outgrowing it? There is such conflicting advice everywhere: keep her exposed to the allergens, but only slightly vs. total avoidance; probiotics; vitamin D supplements… If you have ANY advice or resources to point me toward I would greatly appreciate it!
The reason your dtr is getting allergies has to do with inflammation, so the blanket advice all allergists would give if they were educated in nutrition would be to avoid the most pro-inflammatory foods: Veg oils and sugars. Deep Nutrition devotes one chapter to each, and a third to the harms of inflammation on the collagen in our bodies.
Thank You ! Back to basics, that is more or less where I am now.
I did not have the priveledge to read your book. I have Celiacs Disease, was diagnosed too late, but in time ! The main problem for Celiacs is, what to eat ? Why ? For 1, gluten hides everywhere – you think you are gluten free just to discover you are not. 2ndly ”gluten free” marked products are mostly marked on a scale and could actually still contain gluten – I get sick on contamination & also on ”gluten free” products. I want to know, your book, when you wrote it, did you think of people having a fast metabolism ? people with an O bloodgroup ? for exmp. I am always hungry (typical Celiac). Vegetables does not make me full. Being stressed (typical Celiac) I easily have to much acid (typical O bloodgroup) in my stomach – meat helps me alot, vegetables alone does not help-I ve tried it! My personal opionion is that one person with Celiac could not be put in a box with all other Celiacs when it comes to diet. There is so many different needs & food could assist. We need guidelines what to eat for what condition. I love carrots and sweet potatoes and all of a sudden i’ve lost my taste! Now I discover that Vit A is not good for one with damage to the villia? Help ?
Insurance usually covers a consultation with a dietician, which, while not necessarily going to help you with the underlying cause (dieticians unfortunately tend to promote pro-inflammatory oils and fats, and excessive carb) you will get clear guidance on how to avoid gluten. For the rest I suggest you read more about ancestral/traditional diets and not focus on fad diets.
Thanks Dr Cate. A very interesting video. I have celiac sprue and also have developed a severe lactose intolerance. My intestines were badly damaged- the endoscopy photos were shown to me. YUK. I also developed gall bladder problems and had an attack while traveling.
I was doing better for almost a year but have recently started symptoms as if I were still eating gluten which I am not. I have such a limited diet already and its depressing. Suggestions?
What tests should I ask my Dr. to run to see if I have Celiac?
The best site I’ve seen on this is here:http://www.celiac.com/categories/Celiac-Disease-Diagnosis%2C-Testing-%26amp%3B-Treatment-%28Gluten%252dFree-Diet%29/
Dr. Cate, About four years ago I had a blood test done and the nurse practitioner who ordered the test said I had a gluten intolerance and should not eat it, I’ve followed her advice, but she moved practices so I havn’t had any further testing for gluten. The past seven or so months I have been getting a rash on my lower legs, a rash that turns very sore, kinda of scabs and then heals. Should I be tested celiac? And what exact tests should I get done?
There are many reasons for rashes, including the most common: eczema. It would be best to work with a new practitioner to sort through all the numerous possiblities. Meanwhile, you may want to familiarize yourself with the principles of anti-inflammatory diets at Trimprogram.com and in more detail from Food Rules: A Doctor’s Guide to Healthy Eating.
I cut all gluten out and any Time I eat it I’m very I’ll. Heart beats fast, sweaty, insomnia. What explains this?
You very well may have a kind of allergy to it.
My 10 month old has had eczema and a constant diaper rash, almost since birth. My ND is having us tested for food allergies (something I’ve previously scoffed at because of it’s seemingly “fad” nature). If we find that we have produced antibodies to certain foods, how long do you recommend cutting those foods out to allow for healing?
After paying attention to my diet and when her rashes would flare up, I’m suspecting dairy AND wheat. Really not looking forward to cutting them out. I love milk
A good allergist will advise you that antibody testing is meaningless without a corresponding clear correlation between food intake and symptom development. The time to healinig would depend on a wide number of variables.
Can the testing come up inaccurate? I did an Elimination Diet to find correlations and after cutting out ALL top ten allergens, and the eczema subsided considerably, however, general diaper rashes remained (and I was starving). When I started reintroducing foods, it was really tricky to pinpoint which was what. I also struggle with acne (age 28) and it cleared up as well, but is back. Could it be something as simple as cutting my carbs/sugar and not an allergy at all?
Testing is notoriously inaccurate, and any honest allergy specialist will tell you this before you undergo testing. I’m sorry to say that I see a great deal of salesmanship happening. Simply cutting carbs and sugar, getting good fats and avoiding bad (see Deep Nutrition, Chapter 8 if you need help with that) can work near-miracles for your skin.
Dear Dr Shanahan, This article is the best composite of about a 4′ high pile of books and research papers that I have read to date. And because of your books my world is a better place. Thank you so very much, Bill
Do you recommend Matt Stone’s resources on digestive health/diabetes? I just found his website and see he’s going to be featured in the same Paleo Summit as you. My IBS seems worse since going low carb (GAPS) and I’d like to get back to where I was before…not afraid to eat. Thanks…
I think I found my answer…I’ve been eating insoluble fiber without soluble fiber. I’ll add squash back in. Thank you again for sharing your research with us.
Please let us know how if it works!
Kris, Grains are just seeds, and starchy veggies like squash and potatoes are tubers. So other seeds and other tubers will get you what you need. By switching out wheat for pumpkin seeds or nuts, and potatoes for carrots or radishes, you are trading in a seed or tuber thats higher in carbs to one that’s lower.
When cutting carbs this much, how does a person get enough fiber to help with the resulting constipation?
Jennifer
I recommend her website to my patients w/ GI issues because if if we both ‘get’ inflammation our diet advice should be very similar. I haven’t had time to properly digest her book, though :–)
I also am on the GAPS diet and suggest reading Dr. Natasha Campbell’s book : Gut and Psychology Syndrome. Many people on that forum have also read Deep Nutrition and rave about it (as I have too). You both share similar views on digestion/gut flora and diet. Dr. Campbell also agrees that many of the conditions you state are all from the same root problem: messed up gut. You two would make a killer dietary team!!! 🙂 GAPS can supposedly clear up celiac, but I don’t understand nutrition enough to understand the differences in how both of you go aobut doing that, so I don’t have comments. I do respect both of you and your work very very much! Love this blog and book! Can’t wait for your new one to come out!
Ferris
I think someone has gotten you confused. Histamine is not produced by probiotic bacteria. It is produced by your body’s immune cells in response to infection by pathogenic bacteria.
Hi Dr. Cate,
very good article!
But there is one thing I cannot figure out: What kinds of probiotics can I get into my diet while being gluten, dairy and histamine intolerant at the same time? From my understanding, as soon as a food is fermented, it becomes high in histamine. Is there anything else?
Thanks,
Ferris
Neil
VERY important question. The answer is YES, I believe the sort of sequence of events take place to render someone allergic wheat as to casein as to soy etc. Whether you get rashes, arthritis, neurologic problems, or other issues depends on a combination your genetics and the exact cross-reactivity between antibody and your tissue.
Hi Dr Cate
This is a great article and really ties in with my interest in Molecular Mimicry and Multiple Sclerosis. I think it seems to be quite a plausible explanation for the auto immune response – as you point out in your blog most other theories dont appear to have a consistent hypothesis. I am curious to know if this theory could be expanded to the casein protein – I find it interesting that both my daughters were breast fed until about 12 months and then when put on dairy both developed Ezcema, another auto-immune response.
Fabulous information.
Dr. Cate,
Put up a “share” button for facebook, if possible. I believe this will facilitate traffic.
Thanks,
Wes
Pam
What you describe about the starch molecules being long is true of all starchy foods, so by that definition alone you can’t pick out potatoes as being significantly different from rice or wheat. When it comes to carbs, the dose makes the poison; it’s about the amount you take in. Based on my clinical experience and understanding of our metabolic pathways, at this time I feel over 100 gm per day is too much carb for anyone. Depending on what other medical conditions a person has I sometimes suggest cutting carbs down as low as 20-40 gm per day.
Thank you Dr. Cate! I must admit a little confusion about rice and potatoes referred as safe starches. Are you familiar with the GAPS diet? Dr. Campbell-McBride says that all grains and some root vegetables (potato) are very rich in starch. Starch is made up of huge molecules with hundreds of monosugars attached and because of its complex nature, most of it goes undigested. Thus a food source for pathogenic flora. When it is digested, maltose is produced. In a person with abnormal gut flora, the enterocytes are not able to split double sugars so the maltose goes undigested, etc. etc.
More details are in the Gut and Psychology Syndrome book pages 101-102,
Based on that data, it seems like rice and potatoes are not a safe starch for those with inflamed intestines.
Help!! 🙂 Thanks, Pam
Thank You!