Menopause Symptoms Weren’t Always Common In the early 2000s, I was living in Kauai and…
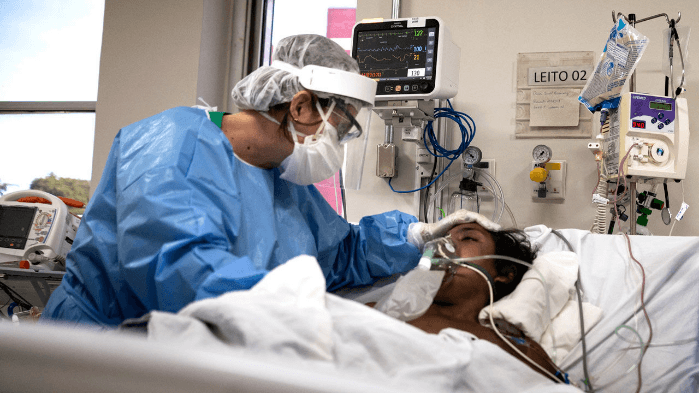
Is the Coronavirus Racist?
Table of Contents
10 Minute Read
Are you scientifically minded?
Here’s a test: Let’s say that wherever you live it rains every Wednesday afternoon, and only on Wednesday afternoons, for five years straight. Are you curious about why that might be? If so, that’s great. Scientists are naturally inquisitive. Do you understand the idea that correlation (rain and Wednesday afternoons in this case) does not equal causation? Of course, you do. But given the fact that it’s been five years of this pattern, wouldn’t you feel compelled to at least investigate whether or not there is indeed a causal relationship between Wednesday afternoons and rain or between some underlying causative mechanism that might somehow be causing both Wednesday and rain simultaneously or that, as mathematically improbable as it may be, this extraordinary pattern may indeed be merely coincidental?
This article is continued below...(scroll down)
If you caught the gist of what I just said. Congratulations! Here’s your honorary Ph.D. in critical thinking.
Just as with the Wednesday rain, some patterns are so unlikely to be mere coincidence that they compel investigation. According to a recent Brookings institute article citing the CDC, African Americans (and other minorities) are at twice the risk of death as a result of COVID infection than white folks—just as they are at twice the risk for diabetes and a number of other metabolic diseases. Metabolic disease is the most common cause of disability and death, so we’re talking millions of lives lost, year in year out. This pattern, in my view, warrants serious investigation in the hopes of shedding light onto an underlying cause that we can all do something about immediately, regardless of race, age, etc.
Conventional Wisdom Creates a Dependency Spiral
My research has revealed that there appears to be a general consensus among leading institutions that the best current explanation for this stark disparity in COVID-related deaths can be traced to things like income, education, type of job and, in the words of the Brookings Institute, “less access to health care or greater prevalence of co-morbidities such as hypertension, obesity, diabetes, and lung disease – which in turn reflect broader racial inequalities.”
The Brookings Institute cites the reality that “Blacks, relative to Whites, are more likely to live in neighborhoods with a lack of healthy food options, green spaces, recreational facilities, lighting, and safety. These subpar neighborhoods are rooted in the historical legacy of redlining. Additionally, Blacks are more likely to live in densely populated areas, further heightening their potential contact with other people.”
If you look into the language used when leading institutions explain away the vast disparity of the incidence of type 2 diabetes between African American’s and whites, you’ll hear similar language: “Disparities in income, education, health literacy, and access to health care may result in otherwise preventable (or treatable) cases of diabetes. And for some, cultural factors….”
The muddled conversations dancing around the rampant epidemic of type 2 diabetes also tends to include phrases like “genetic factors.” This “Sorry, folks. It’s your genes’ fault” approach, whether based in good science or no, may, I fear, rob a little hope from African Americans and other minorities struggling to embrace a proactive mindset because it suggests that a) the problem is ultimately with you and b) that problem is intractable, at least in the short term, as in, “Change your genes. Win the lottery. Starve yourself and lose weight. Live in a great neighborhood filled with parks and opportunity where the sun shines all the time. Otherwise, deal with twice the number of deaths.”
Think about it: Disparities in income. Disparities in economic opportunity. In living conditions. In safety. A genetic predisposition to obesity and diabetes. What do all these things have in common? Answer: They’re all things for which there is no simple and immediate remedy, as much as we all wish there were.
Focusing on these factors to the exclusion of actionable dietary change amounts to a lockdown on the status quo.
What if there were something people of all incomes and population groups could do to bolster their metabolic health and reduce their risk for COVID and diabetes and heart disease and the rest? There is! There’s something we can do, all of us, starting tomorrow, that evidence strongly suggests could have at least some impact on our vulnerability to having a deadly, hyperinflammatory response to an infection with the COVID virus—getting soy oil and other vegetable oils out of your diet.
The logic is straight forward. All credible (and some no-s0-credible) authorities agree that, just as with type 2 diabetes, diet and nutrition are playing a major role in the COVID epidemic. When COVID infects someone with an impaired metabolism, it enjoys a free run, from the initial viral load that enters the body to throwing the otherwise measured inflammatory response into a deadly full-out panic.
Junk food is a metabolism killer. We know this. And since Harvard and Tufts and the CDC and the ADA all refuse to define precisely what junk food is, I will: foods containing significant amounts of high- PUFA vegetable oils are junk food, end of story. Well, with a small postscript: sugars and refined flours make PUFA’s effect on your metabolism even worse. How they work hand-in-hand to destroy your health deserves another discussion—or a quick read of my latest book The FATBURN Fix.
It is undisputed that African Americans, due to economic inequalities, have, as a consequence, less access to real food and more dependency on convenience food, whether from a fast food joint or a BOGO at the local grocery store.
Twice the type 2 diabetes. Twice the rates of kidney failure. Twice the rates of amputation. Twice the rates of vision impairments. Twice the deaths from these and other complications of metabolic disease. At least twice the deaths as a result of a hyper-inflammatory immune system response from COVID infection. Twice the dependency on cheap, seed-oil rich junk food and the two-fold daily insult to their metabolisms.
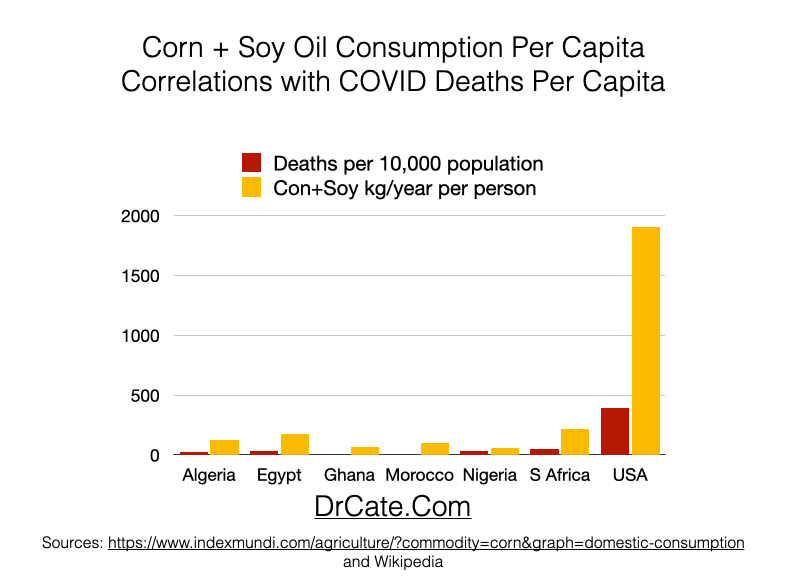
As you probably know, I’ve been saying vegetable oils are our public health enemy #1. If I could post photos of the Hateful 8 in post offices across the country, I would. Not a big fan. Here are some things I do think are good for our health: Nutrient-dense foods. Green beans growing in sunlight in your backyard from soil you fertilized with chicken poop from your neighbor down the street. Chefs who spend more on quality olive oil, from a known source, even though most of their customers won’t ever know how their health was being protected. The ethical treatment of animals. In stark contrast, my experience has shown me that others are quick to grab their saber and leap to their feet to defend vegetable oils.
There are folks who agree with me and folks who don’t.
One group jumps to the defense of highly polyunsaturated vegetable oils, seemingly supporting the idea that we’re not yet eating enough of this stuff! And they’re in respected company, after all, Tuft’s Friedman School of Nutrition and Policy, and nutrition experts from Harvard and Yale are unequivocal on the message to consume more PUFA. If they’re right, they could further contend that their message is of greatest benefit to lower-income families. After all, convenient processed foods and fast foods that are easy to find even in the worst food deserts—were talking Doritos, fast-food french fries, KFC, etc.—are loaded with this stuff. And they’re cheap! How great is that?
The second group seems more given to take on the homework of actually reading about this subject for themselves, rather than aligning with authority figures without question. Many of them have taken action by getting these oils out of their lives and have enjoyed extraordinary health benefits as a result (or at least what they deem to be a causal relationship rather than mere coincidence). I contend that the “authorities” who generate dietary recommendations have shamefully failed the American people, and economically disadvantaged families in particular.
Politically Correct Nutrition Deepens Health Disparities
To the defenders of high PUFA vegetable oils, I have but one request: State plainly and publically where you stand on our current, already historically high consumption of high–PUFA vegetable oils. Do you think we have just the right amount of vegetable oil intake, not enough (as Tuft’s University says), or that we should consider limiting our exposure?
But please realize that your opinions, whether well researched or not, have consequences to everyone you influence. It is Wednesday afternoon right now. The rain is pouring from the sky, in the form of Coronavirus, and I have suggested a likely cause for the intensity of the virus’ threat to the health of Americans, and why that threat is even greater for disadvantaged Americans dependent on cheap, pro-inflammatory foods. Reducing our intake of these things as much as our individual economic situation will allow is a way each of us can build a shelter to get out of the storm.
The rich, the institutionally empowered, the tall white men in lab coats with tales of rowing crew and fraternity pranks have been running the conversation about what we should and shouldn’t eat for more than half a century. We’ve heard their “don’t be so fat” message for decades. More exercise. More fruits and vegetables. More whole grains. It didn’t work out for the American people. And for poor folks, it’s been a disaster—a pandemic of misinformation.
Their claims have failed us—working class Americans most of all. It’s time for new voices.
Recent Posts
Hidden Metabolic Disorders Allow COVID-19 to Kill “Healthy” People
This Post Has 10 Comments
Note: Please do not share personal information with a medical question in our comment section. Comments containing this content will be deleted due to HIPAA regulations.



















So, to be a slow carb it needs to be intact, not pulverized into flour. But at least what you’re getting is going to be a more nutritious version of wheat it sounds like.
Dr. Cate,
I just purchased your book and am loving it. I do have a question about wheat. I know it is very difficult to find a good quality wheat but I have found it. It is called West Mountain Wheat. I have talked to the owner and he said another great thing about their wheat is that they grind it in a very slow process in a mill that has been around for over 100 years so it keeps all the good and is not heated. I have bought their flour and their wheat also and grind it myself.
From your book you need to have slow digesting carbs. This would qualify as slow-digesting carbs? Is that correct?
Hi Dr. Cate!
I am an administrator for a healing center and head of their nutrition program. We do blood chemistry analysis and I am looking for guidance to make sure I am ordering the correct lipid profile test. I am currently shopping for labs and we are not necessarily going to be using Lab Corp. Thank you!
Hi Dr. Cate. Thanks for bringing our attention to yet another inequity in our culture.
I’ve got a question about industrial seed oils in body products like lotion. How does spreading canola oil all over our body when using one of these products affect us? Does this produce any of the same bad effects as ingesting the oil?
Hello Dr.Cate,
I have read both your books, Thank you so much for the great info. Your work is really appreciated. I am sorry to bother you, but if you can find the time to answer it would be much appreciated.
My baby is staring kindergarten soon, and they are obligated to bring one fruit each every day. I want to further my issue with this to the kindergarten and even higher up in the system, on page 223-224 in your book Deep nutrition you mention the effect of sugar on kids and their “reward system/behaviour”. This has also become a real issue with family memebers who gives him bad snacks and think we are stupid for not letting him taste the “good things(food). Sadly, this is a common issue I assume.
If I was as professional and well read as you, how should I further this info so both kindergarden and hopefully the system will change, do you have any tips in that regard?
Thank you so much for your work, you are truly our “rockstar”.
Kind regards
Epcot fam.
Hi Dr. Cate.
In the last six weeks, I read both of your books. I completed Phase I in a month and now I have just started Phase II for the past 2 weeks. I am following your program very strictly but I am really fine with slowly progressing to feeling better and losing weight.
I am really surprized at something. I am 52 and have been in perimenopause for 5 years. But I just had 2 periods in a regular 28 day cycle. That hasn’t happened in years. Also, I’ve lost 10 pounds in 6 weeks. I don’t really understand all the changes that are happening to me so “quickly.” I’m kind of spooked. I really don’t want to lose weigh in an unhealthy way.
But on the other hand, I feel good. I have more energy. When my stomach growls and I say, oh, I’m hungry, let’s eat in a hour or so. My stomach stops growling, I eat an hour later and life is good. I don’t have the hypoglycemic jitters or hangry feelings. I drink water like crazy because my body craves it, not just because you say to do it.
So many of your posts are about explaining the benefits of your expertise. I’m experiencing a lot of these changes and just want some reassurance that this is “normal.” Thank you ahead of time for your response.
Lecithin, probably, right? Not quite and not used in the same amounts. Check the post on the topic here: https://drcate.com/are-prod…
Good almond milks should be sugar free and the fewest ingredients. But almonds are better !
Hello Dr Cate, two quick question . Is sunflowers lectin as bad as sunflower oil? Also are there any almond milks you recommend?
I would agree that it’s best to avoid FL. We have always installed RO systems in at least one sink to use for all our drinking water.
Hi Dr. Cate. Since I read your book Deep Nutrition 3 years ago, I have dramatically changed the foods that I eat and I trust your insight over others on the Web, which is why I’m asking the following question. A Youtube video by Dr. Josh Axe “Top 10 Toxic Foods and Top 10 Healing Foods” puts tap water at #10 on the toxic list because, he claims, medical studies have shown that the fluoride in tap water kills off probiotics in the gut. I have looked but couldn’t find any discussion by you on this topic, so I hope that you can address this. Thank you.