Most nutrition experts claim that the majority of evidence shows seed oils are healthy. But that evidence is not real. Most nutrition experts overlook, or make excuses for, the selective use of flawed, self-reported dietary data that makes seed oils appear beneficial.

Hidden Metabolic Disorders Allow COVID-19 to Kill “Healthy” People
Table of Contents
- This article covers
- Why coronavirus is “like a flu” but also worse than scientists could have predicted
- Why coronavirus can cause lung failure (ARDS) in seemingly healthy adults
- Underlying metabolic conditions predispose people to ARDS
- Most of these conditions are related to high-PUFA seed oil consumption
- How PUFAs promote ARDS
- Simple action points to improve your metabolic health
- The scariest aspect of COVID-19 is its ability to incapacitate and kill seemingly healthy people.
GOOD NEWS! Physical copies of Deep Nutrition and The FATBURN Fix sold out from Amazon but ebooks and audiobooks are still available. Deep Nutrition is available from BooksAMillion.com and The FATBURN Fix is available from Barnes and Noble. Food Rules is available in all formats on Amazon.
This article covers
-
-
-
Underlying metabolic conditions predispose people to ARDS
-
-
How PUFAs promote ARDS
-
Simple action points to improve your metabolic health
The global COVID situation started out on a note of distrust and panic. Early on, experts were saying COVID 19 is “like a flu” but meanwhile a video from a doctor working in China started circulating warning of a serious SARS-like virus causing pneumonia and respiratory failure, followed by what appeared to be a government cover up. Then the man died of the disease he was warning us about.
So why did he die? And if COVID-19 is SARS-like, why were some people saying it’s “just a flu”?
The flu is actually quite serious
Back in 1917, the so-called “Spanish flu” influenza pandemic killed nearly 100 million people, roughly 6 percent of the global population. Nothing like that has happened in modern times thanks mostly to better identification and intensive care, but even today, the flu is the most common cause of respiratory failure in the world.
The flu is highly contagious and can cause a pneumonia and that pneumonia can morph into a deadly lung condition called ARDS (for acute respiratory distress syndrome, which I’ll discuss in more detail below). This year the flu has killed nearly as many people as COVID-19, current estimates range widely from 24,000 – 63,000, and this is not a particularly bad flu year.
This article is continued below...(scroll down)
COVID is like the flu in that it also is highly contagious and can cause a pneumonia that can morph into ARDS. Deaths from COVID-19 now approach 80,000.
The reason it seemed like some were downplaying the seriousness of COVID, by saying “just a flu” for example, is that it’s not fundamentally a lethal infection. The COVID-19 virus is far less deadly than something like a bacterial meningitis or Dengue. The reason this virus is killing more people in the USA than the flu virus is that fewer Americans have been exposed to anything like this virus than have been exposed to the flu. Exposure to the flu each year promotes some natural immunity, in addition to any immunity we can get from flu shots.
Some of us have likely also been exposed to a COVID-like virus, and that would mean some of us may have enough natural immunity that if we were to be infected with COVID we’d have a milder course or perhaps even no symptoms at all. But we have no way of knowing who has such immunity at this point since there’s no antibody testing available at the moment. The testing that’s being done identifies the virus itself, not immune-generated antibodies to the virus.
The point is, the number of us with natural immunity to COVID-19 is lower than the number with natural immunity to the flu, and there’s nobody with vaccine-induced immunity to COVID. Thus, even though the virus itself is not particularly deadly, people who have no natural immunity and who are exposed to COVID are likely to get sicker than they would have done if they’d been exposed to the flu virus instead.
And a proportion of those who do get sick with COVID-19 will die.
The scariest aspect of COVID-19 is its ability to incapacitate and kill seemingly healthy people.
What would have given scientists the ability to better predict how serious the virus would become has nothing to do with virology. It has to do with metabolic health. More to the point, a lack of metabolic health.
We all know that the percentage of Americans with obesity and diabetes keeps going up every year. We also know that obesity and diabetes are two of the common underlying metabolic conditions that make COVID more severe and potentially lethal. But what most folks don’t know is that the same factors causing the obesity and diabetes epidemics are also affecting those among us of normal weight and without other chronic illnesses. In other words, just because you’re not obese or diabetic or taking no medications does not mean you’re metabolically healthy enough to fight the virus effectively. This hidden epidemic of undiagnosed metabolic disease makes apparently healthy people as likely to get severely infected and potentially even die as those with obesity and diabetes.
Most doctors don’t know enough about metabolic disease to properly identify people at risk. Without proper training in metabolic health, few doctors are equipped to explain why younger, normal weight people with none of the more obvious metabolic problems are being affected by this virus. Thus, Li Wenliang, a 33 year old non-obese, non-diabetic doctor working in Wuhan didn’t recognize his own risk, and ended up dying tragically from the virus shortly after recording his now infamous video.
I’m going to discuss how to properly identify your own metabolic health again below. But first, I’d like to highlight the inverse relationship between deadliness and contagiousness. When a virus progresses rapidly and makes people so sick they need to lay in bed or it actually kills people the virus actually can’t spread as far as if it were a milder infection. In other words, this virus has spread around the world so effectively in part because it is not an inherently deadly virus. A big reason it’s spread so fast is related to the fact that CVID-19 symptoms can be so minor that they often go unrecognized, especially in kids.
Coronavirus causes minor cold symptoms in kids
The coronavirus enters human cells by way of a spiked protuberance that is designed to penetrate something called an ACE-2 receptor on human cells. Kids don’t have as many of these in their lungs as adults do, but they do have them in their nasal passages and throats. So when kids get coronavirus, it’s more likely to cause a runny nose or a sore throat and never get into their lungs. Kids with runny noses and sore throats really should be tested for the novel coronavirus, in my opinion. But so far they’re not being tested.

The fact that kids don’t get seriously ill and don’t get tested but nevertheless are loaded with viruses makes them efficient carriers of the virus. Unlike the common flu, where kids and adults get very similar symptoms, it’s not obvious that kids have coronavirus so they can go around spreading COVID-19 and nobody has a clue. It’s a very sneaky strategy that this virus has perfected.
The ability to spread rapidly within a population is required for a virus to become a pandemics because, by definition, pandemic viruses spread fast enough that they can impact the entire world at the same time. Rapid spread is not what makes it deadly.
Why COVID-19 can be deadly: Pneumonia versus ARDS
If a bacteria or virus is able to enter cells of the lung, that enables it to cause a pneumonia.
The seasonal flu commonly causes pneumonia. When people over the age of 85 get pneumonia, they are 16 times more likely than those just a little younger, aged 65-69, to die from influenza. This is mostly thought to be due to the fact that very aged lungs are very inefficient compared to even slightly younger lungs, so just a little bit of infection tips them over the edge and the person cannot get enough oxygen. It’s also partly to the fact that our immune system also gets slower and weaker as we age. Very young children are also particularly susceptible to pneumonia and more frequently also die from the flu because their immune systems are also less efficient. This is partly because they’ve rarely or never been exposed to the flu and/or flu vaccines than older children and adults, and so have build up less of an antibody response.
The coronavirus is the virus that causes most of the colds folks get every year, and very few colds ever lead to a person getting sick with pneumonia. Why is COVID-19 different than a typical cold-inducing coronavirus? As you read above, the virus gets into cells by way of their ACE-2 receptors. Since adults have plenty of these ACE-2 receptors in their lungs, we’re laying down a red carpet for COVID 19 to enter our lungs, resulting in pneumonia.
Even though COVID-19 appears to be more likely to cause a pneumonia than the flu, pneumonia is not a death sentence for folks under 85. It’s not usually even serious enough to land younger folks the hospital. Fortunately, the vast majority of the patients with COVID-19 pneumonia I’m personally familiar with were able to stay out of the hospital and stay in bed at home, just as they would with a flu.
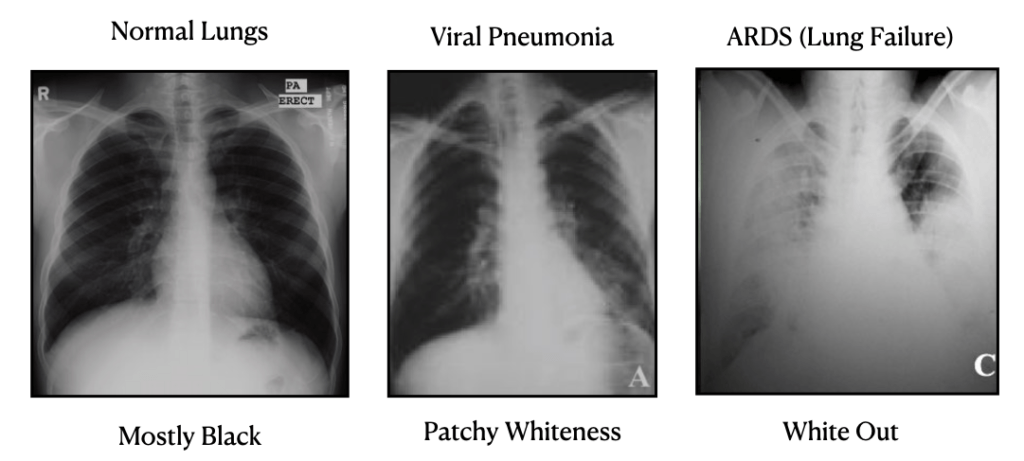
What’s killing most of the people infected with COVID-19 is not the virus itself. The folks needing intensive care and unfortunately quite often dying from COVID-19 have an abnormal response to the virus called ARDS, which, as I’ve said, stands for Acute Respiratory Distress Syndrome.
Acute means it comes on over days or weeks, not months or years. Respiratory means it affects your breathing. Distress means what it sounds like it means (its a bit mild of a term if you ask me) considering people are suffocating). Syndrome means it can come on as part of another illness, in other words it has more than just one cause.
What’s happening when a person develops ARDS is that the normal response to infection is broken. With pneumonia, the immune system attacks only infected cells and causes a little bit of inflammation, which can be seen as a little bit of whiteness on a chest X Ray. With ARDS, the inflammatory response goes completely haywire and fluid starts leaking from the bloodstream into the lungs until a person basically starts drowning in their own liquid serum. A comparison might be the difference between a typical allergy that might cause runny nose versus an anaphylactic peanut allergy response that can be deadly.
Everyone with ARDS needs to be put on a ventilator (a breathing machine) which means they not only need to be in a hospital, they need to be in an intensive care unit (ICU). The whole reason we shut the world down to “flatten the curve” is that we only have a limited number of ICU beds, and the early predictions were that if we didn’t slow down the spread of the infection to reduce the number of folks getting sick all at the same time, the number of people needing an ICU bed would exceed the number of ICU beds available. If that were to happen, we’d have had to chose who gets a bed and who doesn’t, meaning who lives and who dies.
Another option would have been to reduce the need for hospital beds by reducing the number of people prone to getting ARDS. To do that, we’d have to start by having a better understanding of the metabolic conditions that promote ARDS. While it’s too late for this pandemic, there will likely be facing another pandemic situation in the future, and I hope by then we’ll have more doctors who are knowledgeable about metabolic health.
Metabolic Conditions, Many Overlooked, Promote ARDS
It’s clear that not just anyone gets ARDS from COVID. The CDC lists a number of underlying conditions found in 64% of all people who’ve been admitted to the intensive care (shown below). Still, that leaves a sizable 36 percent who would be labeled as ‘healthy.’
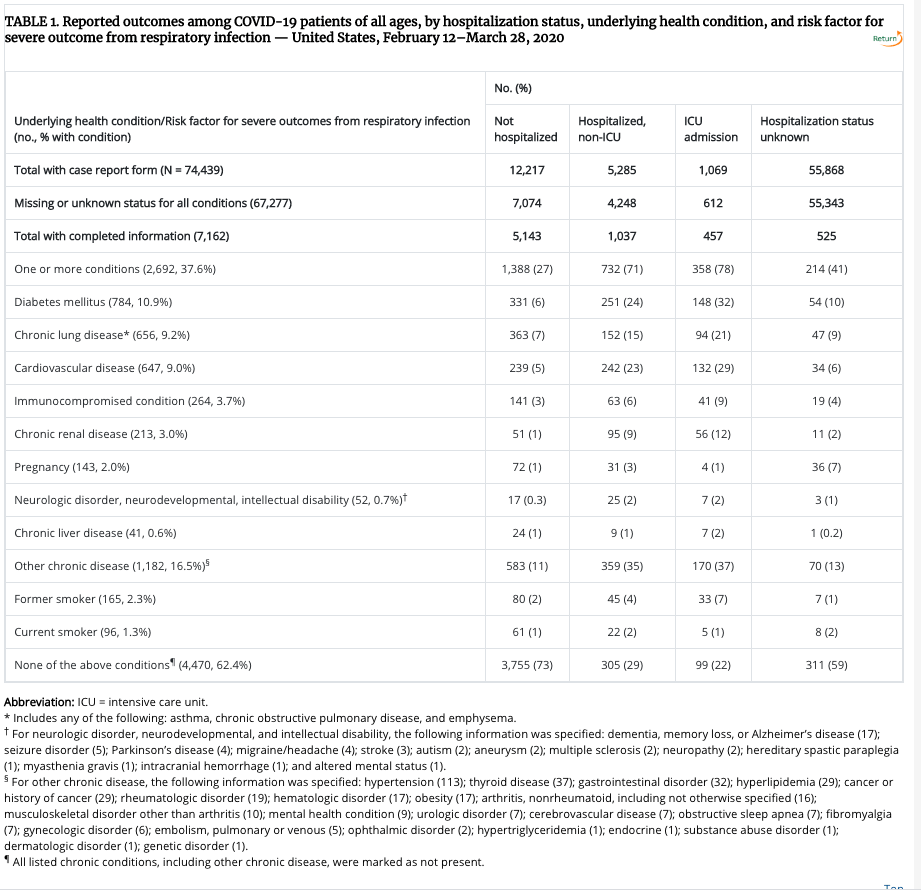
The apparent unpredictability of deadly serious COVID cases makes it seem like being struck by lightening–it could happen to anyone. And that’s part of what makes it so scary.
But that’s not what’s really happening.
People admitted to intensive care units most likely ALL have had an underlying metabolic condition, but the condition wasn’t necessarily diagnosed. Even if the doctors notice high blood sugar readings or abnormal liver function tests they’re more likely to misattribute these findings to the stress response or the infection than they are to consider whether the patient has prediabetes or fatty liver.

Most metabolic conditions are related to high-PUFA seed oil consumption
Whether or not you know you have a metabolic condition, there’s something you can do right away to protect your health. First, lay off the orange juice as a source of vitamin C. You get two times more vitamin C from bell peppers than you do from an orange, so go make a salad (but make your own dressing). An even more important, and more powerful, action you can take is to stop eating high-PUFA seed oils.
PUFA stands for polyunsaturated fatty acid. High-PUFA seed oils are in every sort of junk food, fast food, and processed food. Over the past 110 or so years, our dietary intake of PUFA has increased by a factor of 20, that’s 2000%. (For more information on how to find and avoid high-PUFA seed oils and what fats are the good fats, click here.)

At birth, we have a relatively normal amount of PUFA in our body fat. When our diet is too high in PUFA, the concentration of PUFA in our body fat goes up. At some point, and its different for everyone, the concentration of PUFA reaches a threshold where your body fat does not function properly and you develop symptoms of metabolic dysfunction. The most common symptoms are usually misdiagnosed as hypoglycemia. If you have hypoglycemia, you are on your way to developing a condition called insulin resistance, which is the underlying hormone dysfunction behind type 2 diabetes.
All of the underlying conditions on the list above are metabolic disorders related to insulin resistance or result from treatment of related inflammatory conditions. For nearly two decades, my medical practice has focused on reversing metabolic and inflammatory diseases like diabetes, obesity and hypertension with diet. Over this time, I’ve come to understand that the number one cause of metabolic disease is eating too much PUFA. Of course, it’s not just me, many doctors who specialize in metabolic medicine have come to the same conclusion.
Too much PUFA promotes ARDS
Too much PUFA in your body fat also puts you at risk of respiratory failure from COVID-19.
When you get a pneumonia, your appetite drops off to next to nothing and you’re not generally going to be eating. When you’re not eating, your body will release body fat into your bloodstream (in the form of free fatty acids also called non esterified fatty acids, or NEFA). If you’ve been eating enough seed oils to develop one of the underlying conditions listed above, then a dangerously high proportion of the fatty acids in your bloodstream will be PUFAs. PUFAs are dangerous because they react with oxygen in ways that lead to massive amounts of inflammation.
Inflammation makes the difference between a case of pneumonia that you can recover from on your own and a case of ARDS that lands you in intensive care.

What I’m saying is that if there were no such thing as high-PUFA seed oils, and by the way there wasn’t before the industrial era, then this COVID-19 pandemic would not be so deadly, truly ‘just a flu.’ Albeit, a really bad one. But there’d be no need to ‘flatten’ a curve, kids would still be in school, there would be a normal amount of toilet paper on the shelves and we wouldn’t be at home worried about how we’ll survive a global economic depression.
If your doctor hasn’t told you about the dangers of high-PUFA seed oil consumption, that’s because only the most up to date, knowledgable doctors who are interested in metabolic medicine even know what PUFA means, not to mention why it’s harmful. Our medical education does us the disservice of convincing us we learn the truth about nutrition.
Fortunately, more and more doctors are questioning the current nutrition and preventative medicine standards and getting up to speed on the science of metabolic health. And that means more and more people with metabolic conditions that put them at risk of everything from heart attacks to cancer are being told of the risk and taking steps to get healthy. Thanks to hundreds of metabolically minded MDs around the world writing books and running clinics, dramatic health turnarounds like diabetics who get off insulin and people headed for knee replacement surgery running half marathons are becoming possible every day.
ACTION POINTS
- If you’re just beginning to learn about metabolic health, a great place to start is listening to podcasts. I’ve been fortunate to have been invited onto some of the best, and you can learn more about that on my youtube channel podcast playlist.
- Eliminating seed oils is the single most important thing you can do to improve your health. Here are the places they commonly seep into your meals
- Breakfast: Muffins, donuts, granola bars and breakfast bars
- Sample fast&healthy breakfast: Yogurt topped with your fave nuts/berries | avocado toast on sprouted grain bread
- Lunch: Salad dressings, fried foods and sandwich condiments like oil and mayo (not mustard or ketchup)
- Sample fast&healthy lunch: Salad with olive oil and balsamic dressing | melted cheddar on corn masa tortilla (these are usually oil-free) topped with green salsa
- Dinner: Take out, sit down restaurants and frozen dinners, especially the starchy stuff (i.e. tater tots, breaded meats)
- Sample fast&healthy dinners: Rotisserie chicken (you can buy in most grocery stores) & cole slaw you make with an avocado oil mayo | Instant pot butter chicken (my favorite recipe here) over steamed cauliflower
- Breakfast: Muffins, donuts, granola bars and breakfast bars
Further Reading
For more on the connection between PUFA and inflammation, here’s a quick and dirty (and free) summary of my first book, Deep Nutrition: Why Your Genes Need Traditional Food
For more on the connection between PUFA and metabolic health, my latest book, The FATBURN Fix.
How to Find a Metabolic Health Doctor
Since it’s not a recognized speciality, we belong to several grass roots organizations. Search for “Low carb MD” “Paleo MD” “Paleo Doctor” and “Keto MD”
The best single resource currently is https://www.dietdoctor.com/low-carb/doctors/find (you may have to sign up for a free version with your email)
For more on the PUFA-ARDS Connection:
Surfactant phospholipids: synthesis and storage.
https://www-ncbi-nlm-nih-gov.prx.hml.org/pubmed/1566854
Pulmonary surfactant, a complex consisting of 90% lipids and 10% specific proteins, lines the alveoli of the lung and prevents alveolar collapse and transudation by lowering the surface tension at the air-liquid interface.
Dipalmitoylphosphatidylcholine constitutes approximately 50% of the surfactant lipids and is primarily responsible for the surface tension-lowering property of the surfactant mixture.
Surfactant phospholipids are produced at the endoplasmic reticulum of the alveolar type II epithelial cells.
The characteristic lamellar bodies in these cells serve as storage depot for the surfactant before this is secreted onto the alveolar surface
Five Decades with Polyunsaturated Fatty Acids: Chemical Synthesis, Enzymatic Formation, Lipid Peroxidation and Its Biological Effects
https://www.nature.com/articles/pr1986144
Adding linoleic acid oxidation products stimulates further oxidation in lung mitochondria and microsomes. In article quote “…Lipid Peroxidation Stimulated by Linoleic Acid Hydroperoxide of Rat Lung Mitochondria and Microsomes”
Surfactant protein d, a marker of lung innate immunity, is positively associated with insulin sensitivity.
https://www-ncbi-nlm-nih-gov.prx.hml.org/pubmed/20086254
Diabetics have lower levels of surfactant protein d than non diabetics, and weight loss in these patients lowered their surfactant protein d further.
This is as you would expect IF 1) PUFAs oxidize surfactant protein d thus reducing levels and 2) Weight loss in DM2 releases more PUFAs and further shifts the FA composition within the type2 alveolar cell towards oxidation.
Altered Lipid Composition of Surfactant and Lung Tissue in Murine Experimental Malaria-Associated Acute Respiratory Distress Syndrome
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4666673/
Inflammation and increased endothelial permeability are important features of both human and mouse MA-ALI/ARDS malaria associated lung injury. Oxidative degradation of lipids results in the accumulation of reactive aldehydes, such as malondialdehyde (MDA) and 4-hydroxynonenal (4-HNE), which are highly cytotoxic [16, 17]. An altered lipid profile and increased levels of lipoperoxidation end products have been found in plasma from patients with ARDS of different aetiologies
Alteration of fatty acid profiles in different pulmonary surfactant phospholipids in acute respiratory distress syndrome and severe pneumonia.
https://www.ncbi.nlm.nih.gov/pubmed/11208632/
PUFA of certain surfactants elevated by 3+ x in ARDS v healthy controls, MUFA not much different, other surfactants are elevated in MUFA but as a percentage elevated less than the PUFA elevations (downloaded PDFto 27 inch mac search by title)
Surfactant alteration and replacement in acute respiratory distress syndrome
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC64803/
Role of hypercoagulability touched on in one of the figures
Increased saturated phospholipid in cultured cells grown with linoleic acid
From https://link.springer.com/article/10.1007/BF02796331
Linoleic acid alters phospholipids
This Post Has 12 Comments
Note: Please do not share personal information with a medical question in our comment section. Comments containing this content will be deleted due to HIPAA regulations.


















vidalista 60 mg dynamic moiety of the medication goes under the classification of a PDE-5 catalyst inhibitor, as the PDE-5 protein is liable for the helpless bloodstream. Tadalafil shows its activity by impeding the working of PDE-5, which prompts stoppage of the breakdown of cGMP into the body.
There death rate from Covid 19 is very low in many countries such as Vietnam and Thailand. Would it be right to assume that the tropical oils have something to do with this or do we assume this area has a high immunity to this corona virus?
Thanks. Is there research on this? I’ve had trouble finding good info on this.
Common question! I’ve posted an answer on the page link below:
https://drcate.com/list-of-…
Scroll down to: What about high-oleic sunflower oil, is it better?
Common question. I’ve posted an answer on the page link below.
https://drcate.com/list-of-…
Scroll down to
How long does it take to get the excessive PUFA out of my body?
Hi, once you stop eating seed oils, how long does it take fat PUFA content to clear? And my daughters eat a lot of the vegetarian patties and meat substitutes, all of which contain canola oil. Is there any meat substitute that does not contain this?
I don’t see any distinction made between high oleic vs high linoleic safflower oil. I believe high oleic is healthy and low in PUFAs. Can you comment?
Will do! Thanks Doc!
Glad to hear you are on the war path for your health! That sounds like a good plan given the circumstances, yes. I would also recommend considering additional inflammation fighting supplementation like magnesium oxide 250mg and vitamin D 2-4000 iu, and I am currently working on a post about that. If you subscribe you will get it delivered to your inbox the day it goes out, which should be very soon.
Hi Dr. Shanahan, I heard you on “Dose of Drew” yesterday and I had a question about avoiding seed oils.
After hearing you I separated all my foods into “Those with Seed Oils” and “Those without Seed Oils”. Turns out half my stuff, including the peanut butter (dang!) had bad seed oils.
I’m morbidly obese, in my 3rd year of recovering from overeating for the last 14 years, so I think there’s a lot of stored oils in my adipose tissue. So even if I avoid the seed oils and lose weight I still get them from fat stores. So right now, instead of throwing away the food I’ve bought while sheltering in place, I’m just trying not to double up on foods that do have seed oils in them. So for instance, I have chicken pot pies in the freezer for dinner that have bad oils in them. So for breakfast and lunch I eat the foods that have good or no oils, like the cereal “Total” so I get a daily dose of zinc, (or take a multivitamin). Is that a sound plan do you think?
What do you think about foods with “less than 2%” bad oils?
BTW, this whole situation has put me into “mission mode” and I’ve been losing weight steadily for the last month by rationing.
Thanks for reading, and if you don’t get back (I know you’re busy, and I’m probably imposing) I will not take it personally.
Thanks for the info!
Yes until your body fat PUFA content has cleared. The less you eat, the faster it clears!
Thank you for the insightful info. I am 35 male with possible sleep apnea. I eat well according to your principles and avoid PUFA. According to your post, it seems that I can be high risk?