Take a look in the mirror. Somehow, you've wound up with a gut. We don't…
Going Low-Carb too Fast May Trigger Thyroid Troubles and Hormone Imbalance
Table of Contents

If you’ve been turned on to the low-carb Paleo diet craze, you may have noticed increased energy, better digestion, happier mood, and a shrinking waistline. Good for you. But some folks who’ve taken the Primal leap—particularly those who were previously on a high-carb diet—have been faced with unexpected side effects waving them back to the world of bread, sugary fruits and sweet potato casserole.
Interestingly, these side effects include a wide range of symptoms that are nearly identical to symptoms of severe thyroid hormone deficiency. More interestingly, lab tests often show normal or near-normal thyroid function. More interesting still is that these symptoms seem to only be relieved by adding back carbs into the diet, sometimes upward of 300 grams—a level I consider to be very likely to harm.
Why is this happening? Is it that low-carb simply doesn’t work for everyone, or is something else going on?
This article is continued below...(scroll down)
The low-carb conundrum just so happens to be an issue I’ve been pondering since reading about the controversy over safe starches. Recently, a couple of pieces of the puzzle fell into place that I think add up to at least one explanation for the debilitating symptoms and offer a method for anyone going low-carb to do so without problems.
Here’s what I discovered about those with thyroid problems.
Abrupt Change May Be too Much For the Thyroid
People who run into trouble going low-carb seem to follow a pattern. They follow any number of diets from SAD to vegan before making a relatively abrupt switch to a low-carb (often less than 50 gm) diet. At first they lose weight as hoped, but then, instead of feeling more energetic from their weight loss, they develop fatigue, sometimes accompanied by symptoms of low thyroid function, including cold extremities, hair loss, and digestive problems. Only by consuming more carbs again can they reduce these symptoms.
Because their fatigue and other symptoms are classic for thyroid malfunction, many will get their levels tested, only to come away confused when the tests health practitioners typically order (TSH and T4) come out normal.
Those who get more extensive testing may get a test called reverse T3, or rT3 for short. These are often abnormally high, leaving them to believe they have found the root of the problem. Some are given a prescription for T3 in hopes of regaining energy, and the intervention seems to help, at least a little.
Reverse T3 is a kind of chemical opposite of regular T3, a mirror image compound called an enantiomer. Reverse T3 has opposite effects of T3 and has long been associated with a set of symptoms aptly called hibernation syndrome—fatigue, weight gain, and so on. If you have suffered from severe hypothyroidism, you may have gone through times when you felt like you really just want to crawl away to a quiet place and rest for a long, long while. Your body was telling you to hibernate.

In addition to making our energy go dormant, high rT3 is also associated with increased levels of LDL, often in the 200s.
Interestingly, those who have added carbs back into their diet and have gotten retested find that their levels of rT3 have gone down without additional T3 supplementation. What’s more, if their LDL was high, adding carbs back to the diet also solved that problem as well, completely counter to the idea that carbs drive insulin which increases LDL.
I have to admit that though I have cared for thousands of people following low-carb diets, to my knowledge, none ran into this problem, so I paid very little attention to the issue with rT3. Only when I started reading about people suffering from thyroid side effects from following low carb did I started seriously thinking about that pesky little molecule. I wondered what it was supposed to be good for: Why would nature program our biology to manufacture a compound that seems to do little other than make people miserable and potentially clog our arteries?
The reason low carbing triggers thyroid changes
In doing research on rT3, I ran into a fascinating article on a group of little-understood compounds called thyronamines (pronounced thigh-row-na-meens). The key to understanding rT3, and unlocking the relationship between carbohydrate consumption and thyroid function, may lie in these newly discovered compounds.
Thyronamines have powerful effects on energy metabolism
Studies performed in 2010 showed that injecting thryronamines into the belly cavity or brain tissues of experimental animals cause the following physiologic and behavioral changes:
- Impaired ability to utilize sugar as an energy source
- Insulin resistance
- Lowered basal body temperature
- Weaker than normal heart contractions
- A marked decline in activity (We can’t ask the lab animals, but presumably, this would be induced by what we would describe as feelings of extreme fatigue)
Sound familiar?
Upon injection, the effects begin within minutes and last 8-12 hours.
And here’s the punchline: Thyronamines appear to be manufactured from that go-to-sleep hormone reverse T3. We can’t yet test you for high levels of thyronamines, but in testing your rT3, we are testing for the precursor of thyronamines. And I expect that, when studies are done in people, we will discover that high blood levels of rT3 do indeed correlate with high tissue levels of thyronamines.
I think this research is vitally important and that we will be hearing more about thyronamines in the future. But we are still left with a very important question that remains unanswered: What do we do about it?
For an answer, we can look to nature and find what I call The bear in the woods theory.
Changing from carb-burn to fat-burn demands new metabolic machinery
The bear in the woods theory suggests that it is the relatively sudden change from high carb to low that flips the switch.
Bears are omnivores, just like humans. And, of course, bears hibernate. Understanding the variations of a bear’s diet throughout the year helps us to understand why biology has built into our mammalian metabolism a sensitivity to changes in carbohydrate consumption.
Imagine you are a bear living in Yellowstone national park. It’s late summer, and the salmon runs are gone, the grazing animals born in spring have now grown too fast for you to catch, the grubs under the rocks are all hatched, and pretty much all that’s left, aside from campground garbage, is nuts and berries. Plucking ripe berries off a bounteous shrub is far easier than cracking nuts, so you gorge on berries. In a few weeks, though, the berries are gone, and there’s very little food left. That’s okay, because the abrupt decline in carbohydrate consumption is accompanied by increased reverse T3 and increased production of thyronamines, which makes you feel exhausted. Thanks to all the weight you gained, you are now so well-padded with cushy fat that you think you could just crawl into a cave somewhere and sleep for a long, long time.
Research in humans shows that, just like bears, our thyroid hormones are influenced by major changes in the amount of carbohydrates consumed.
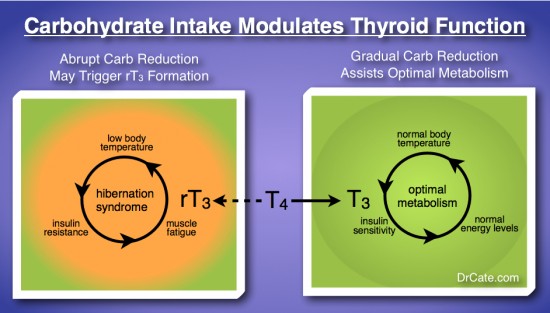
For some, an abrupt decline in available glucose may trigger an atavistic hibernation reflex, which will trigger the conversion of a thyroid hormone called T4 into something other than the normal T3, namely into the reverse form, rT3. rT3 then gets converted into thyronamines and causes all the symptoms of low thyroid function without significant deficiencies of thyroid hormone showing up on lab tests, leaving people to worry there is something incredibly wrong with their hormonal function.
How do you enter fat-burning mode without going into hibernation? The solution is gradual change.
If you have gone low carb successfully, you have accomplished a major change in your metabolism, one that involves turning on scores of enzymes your body has not needed or used for a long time, decades in some cases. Not everyone can accomplish this overhaul in time. Those who can often continue low carb for life with great success. But those who cannot accomplish all the necessary changes flip the hibernation switch, and increase production of rT3 and thyronamines, which causes crushing fatigue and may lead to intense carb cravings in order to turn off the hibernation switch again.
For these people, an easy way to avoid flipping the hibernation switch and reduce carb cravings may be to simply make a more gradual reduction in carbs rather than an abrupt one.
Atkins, who advocates an abrupt switch to less than 20 gm per day, seems to have been aware of this problem, and in fact, in his writing, he warns people they may experience fatigue in the first few days or weeks after going very low carb. Unfortunately, for some people, the fatigue never improves, and they give up on low-carbing altogether.
Instead of giving up, I believe you can try again but next time don’t go cold turkey on carbs. Cut back gradually.
Incidentally, none of my patients reported feeling worse when they went low carb. I suspected it had something to do with the fact that I introduced them to low carbing one meal at a time beginning with breakfast. I made this recommendation simply because I didn’t have time to go over everything with them in one visit. I only had time to give them ideas for one meal, and had them start by cutting carbs from breakfast because that is the time of day we are most able to switch our dormant fat-burn enzymes from off to on.
Bottom line: If you jump into the Paleo (or any low-carb) program and hit a brick wall because of side effects, instead of giving up on low-carbing for good, add back your carbs until you feel better again and then try cutting down again, but go slow to give your body the time to adapt to the idea. This way, your low metabolism can gear up to give you the fat-burning benefits of hibernation without having to take the four-month winter snooze.

This Post Has 201 Comments
Comments are closed.
Note: Please do not share personal information with a medical question in our comment section. Comments containing this content will be deleted due to HIPAA regulations.



















[…] Going Low-Carb too Fast May Trigger Thyroid Troubles and … – Home; Going Low-Carb too Fast May Trigger Thyroid Troubles and Hormone Imbalance […]
[…] Going Low-Carb too Fast May Trigger Thyroid Troubles and … – Hi, I was doing a cyclic ultra low carb diet that (I think) caused my LDL to go up rapidly. After doing a Thyroid test, it was on the low side. […]
[…] Going Low-Carb too Fast May Trigger Thyroid Troubles and … – Hi, I was doing a cyclic ultra low carb diet that (I think) caused my LDL to go up rapidly. After doing a Thyroid test, it was on the low side. […]
[…] Going Low-Carb too Fast May Trigger Thyroid Troubles and … – Hi, I was doing a cyclic ultra low carb diet that (I think) caused my LDL to go up rapidly. After doing a Thyroid test, it was on the low side. […]
[…] Going Low-Carb too Fast May Trigger Thyroid Troubles and … – Hi, I was doing a cyclic ultra low carb diet that (I think) caused my LDL to go up rapidly. After doing a Thyroid test, it was on the low side. […]
[…] Low carb has been all the rage for quite some time. We stumbled onto the whole thing about 3 or 4 years ago when my hubby had some serious health issues. Initially the greatest warning I could find were about ketosis. As time passed I started struggling with some imbalances and I started really digging into it. Turns out, low carb too quickly, too much is really really really dangerous. Ketosis is the least of your problems so take it very slowly. In this article Dr Cate touches on thyroid problems that could be triggered by going low carb too quickly. But go read for yourself. Dr Cate on low carb and the thyroid […]
[…] Going Low-Carb too Fast May Trigger Thyroid Troubles and Hormone Imbalance […]
You specifically mention folks who develop rT3 but have no other blood lab signs of hypothyroidism. What about someone who has hypothyroidism PRIOR to going low carb, then 18 months in, his/her rT3 to free T3 ratio is terrible? I believe all of this was tested prior to 2009 (the rT3 ratios before), but I’m not certain, as I don’t have ready access to those records. That being said, I do have evidence showing TSH issues (and negative antibodies tests – both types) and treatment with T4 medication before I pushed for rT3 testing this time, and got numbers showing that I needed treatment there, too.
I’m an all or nothing person – and always have been. I can’t (easily or successfully, so far) do moderate carbs without flaring up my insulin resistance to the point I faceplant into ALLTHECARBS… It’s frustrating. I started low carb at the behest of my endocrinologist on 1/15/15, aiming for 50 grams of carbs. I was close for that first month, then realized I was closer to keto levels, so I took that leap on 2/18/15. I lost weight steadily until the end of March/beginning of April, and then I started gaining. I’ve managed some of that gain again, but have yet to find my footing solidly again as far as losses. I did take some time off my low carb plan around the holidays (about a total of 30+ days, but not all in a row). Other than random 100 grams of carb days, I’ve been back low carb since 1/25/16, but I’ve not lost more than 5 pounds in that time, though I have gotten back down my previous size jeans I was in prior to going off plan.
I’m just curious specifically how the rT3 issue can be present with and without underlying other thyroid issues – and whether it’s still related to this issue…of needing to up carbs, etc.
[…] Going Low-Carb too Fast May Trigger Thyroid Troubles … – At first they lose weight as hoped but then, … which will trigger the conversion of a thyroid hormone called T4 into something … If you have gone low carb … […]
[…] https://drcate.com/going-low-carb-too-fast-may-trigger-thyroid-troubles-and-hormone-imbalance/ […]
[…] References: – Vreugdenhil, A. C. E., Snoek, A. M. P., van ‘t Veer, C., Greve, J.-W. M., & Buurman, W. A. (2001). LPS-binding protein circulates in association with apoB-containing lipoproteins and enhances endotoxin-LDL/VLDL interaction.Journal of Clinical Investigation, 107(2), 225–234 – Horton, J. D., Cuthbert, J. A., & Spady, D. K. (1993). Dietary fatty acids regulate hepatic low density lipoprotein (LDL) transport by altering LDL receptor protein and mRNA levels. Journal of Clinical Investigation, 92(2), 743–749 – Tosco A et al. Molecular bases of copper and iron deficiency-associated dyslipidemia: a microarray analysis of the rat intestinal transcriptome. Genes Nutr. 2010 Mar;5(1):1-8. http://pmid.us/19821111 – Harvey LJ, McArdle HJ. Biomarkers of copper status: a brief update. Br J Nutr. 2008 Jun;99 Suppl 3:S10-3. http://pmid.us/18598583 – Juan J. Díez, Pedro Iglesias. (2014) Serum cholesterol and triglyceride levels in diabetic patients with subclinical hypothyroidism. Endocrinología y Nutrición (English Edition) 61, 419-425 – N. Silva, O. Santos, F. Morais, I. Gottlieb, M. Hadlich, T. Rothstein, M. Tauil, N. Veras, M. Vaisman, P. d. F. Teixeira. (2014) Subclinical hypothyroidism represents an additional risk factor for coronary artery calcification, especially in subjects with intermediate and high cardiovascular risk scores. European Journal of Endocrinology 171, 327-33 – https://drcate.com/going-low-carb-too-fast-may-trigger-thyroid-troubles-and-hormone-imbalance/ […]
[…] Dr. Cate Shanahan – I’ve referred to this same post a while ago, but I’ll link it again here. She’s part of Mark Sisson’s Primal Advantage program. In this post she describes reading about people that have gone low carb and developed elevated rT3, and thinks this is mainly due to going low carb too abruptly. She says that she’s been able to avoid this problem in her patients by transitioning them to low carb gradually over time. […]
[…] read about a number of hormonal issues taking place in folks that go too low carb, and continue to work out intensely (and even those who […]
Hi,
I was doing a cyclic ultra low carb diet that (I think) caused my LDL to go up rapidly. After doing a Thyroid test, it was on the low side. I’ve added back carbs and will retest LDL soon but I really preferred the effect of low carb (leaning out) what do you think is to low? is 50 grams a day too low or would that be gradual enough to prevent LDL issues? All my other numbers are great CRP, LDL is big and fluffy, particle count low, just not clearing from the blood.
Thanks,
Ben
Paleo is not lowcarb, that is a misconception. Paleo is carb neutral. It means whatever carb level that suits you. Going grain free doesn´t mean going lowcarb necessarily, it just means getting rid of this type of carbs that can trigger inflammation, leaky gut etc. Some prefer a lowcarb Paleo diet, some say that high or medium carb paleo is the best but it is very individual. There are healthy carbs in many other vegetables.
You may want to read some of Paul Jaminet’s work. I too felt like crap on a very low carb diet but after following Paul’s advice I’m finally regaining my health. Good luck.
Hi Dr Cate, I have been following a Ketogenic Diet without dairy and eating mostly oily fish, eggs, avocado – for protein between 60 – 70 g day. Appropriate for my body weight and energy expenditure. Leafy green carbs. In total net carbs below 20g; and coconut fat. Eating in total between 1,200 to 1,500 cals a day. I am not really overweight but have lost nearly 9lbs which I am happy about – presumably some of that ‘water weight’. By adding MCT oil I finally managed to get into nutritional ketosis after 4 weeks of not getting there and cutting way back on the carbs. I never get above 1.3mM using the blood ketone monitor. I have had several days of feeling really well…but now this is my third day of feeling so awful – dry eyed, low body temp despite it being midsummer, can’t think straight, and no energy, also feeling vaguely nauseous. Constipated (I am drinking adequate water). No hunger pangs at all.
I am following this diet because I have intolerances to certain foods, chronic fatigue type symptoms when I over do things – with a feeling I’ve got flu when I haven’t; and because I have blood sugar issues, sleep problems and a mood disorder. Blood sugar and mood has remained more stable, and I have been able to fall asleep very easily, whereas before this diet I was not able to at all. However, as I write to you, I am making a little brown rice to eat now to introduce a little carb back and see if this helps address these immediate symptoms, because I realise I cannot go on another day feeling like this. I am in a dilemma regarding all this! Of course, nothing is as clear cut as things seem; but I am very disappointed that various experts in the field of KD are not pointing out the problems that can happen attempting such a diet and way of eating. I am grateful to Dr Peter Attia for at least mentioning he didn’t honestly know why some women, in particular do not seem to do so well on a KD when pre and menopausal. I am post menopausal and although I took bio identical progesterone in the premenopausal stage, I don’t now, and I never suffered hot flushes. And, now, I am sure, for me, who already had a thyroid that I suspected was not functioning optimally is now seriously in distress.
If I reintroduce some starchy carbs back – less than 100g to start with, no doubt this will take me out of ketosis, certainly as I was struggling to get to ketosis when eating max 20g net carbs. From the way Drs Volek and Phinney describe in their book ‘The Art and Science of Low Carbohydrate Performance’ it seems, to me, they are saying your body either operates by using carbohydrates for fuel OR ketones once the body is no longer ingesting enough carbs, it will then adapt to making and using ketones – which they say usually takes between 1 and 4 weeks…so, I guess I am asking if I am no longer in ketosis, how can my body adapt to a low carb diet? Yet, that is what you are saying, I think. Will this mean I can eventually try to go back to being in nutritional ketosis, or not?
Please advise – I live in the UK and I have friends who are doctors and they are so sceptical of the whole LC thing anyway, and my own doctor would not support me in this. I feel overwhelmed now by feeling I am weakening my already not too strong body and mind. I do not have the money to spend on a nutritionist – and if I did find one it would have to be one who knows about KD and knows of these potential problems and how to address them.
Not to state the obvious but we wrote 2 books and if you have not read either you will learn a lot about what you might be doing wrong.
Hi Dr. Cate! I learned about you from Sean Croxton’s podcasts and I am a big fan of both of you! I myself am an orthopaedic surgeon and now use natural health principles in treating my own patients – thanks to you! Could I get your advice for my wife please? She’s 45 and had radioactive thyroid ablation when she was 18 for Graves disease. She’s been on levothyroxine since then. We have been gluten free for 2 years, but not dedicated paleo tho’. She tried porcine thyroid last december and she went severely hypothyroid over 2-3 months. Her family doc then put her back on levothyroxine and stopped the porcine. Since then, she remains hypothyroid (no blood work to support this…just symptoms). She just doesn’t feel right. She’s gaining weight, has muscular pains and back spasms, dry scaly scalp, cold intolerance, low energy, etc. Any advice? Thank you so much! Jaydeep
If t3 has not been checked that may be an easy fix. Otherwise, make sure her diet is optimized to exclude bad fats and include all Four Pillars and a consultation with a knowledgeable low-carb doc in your area may be worthwhile.
This article explains exactly what I have been going through. May 2012 I decided to go on a low-carb diet, after having exercised intensely for 8 months without changing from my high-carb-low-fat diet– and without losing weight. Within two months I was so lean that my girlfriend begged me to put on a little weight again. But then, at the same time I started feeling extremely tired especially after 7-8 PM, I would feel as if I was half asleep and exhausted. Interestingly, at first I was feeling good, relaxed and not hungry at all when this occurred. But after another month or two of a strict low-carb diet I started feeling really exhausted, plus I started having problems with constipation and insomnia– and during winter I started to gain weight around the mid-section, as well as losing a bit of muscle.
I am now much less strict about my carb intake. I usually eat low-carb meals, but I’m not afraid to eat a small serving of potatoes or white rice once in a while if I start feeling fatigued and brain fog. Usually I will get a surge of energy and high spirit within 30 minutes of eating just one small potato at night– this has also helped me sleep much better.
Anyway, thanks for the article, I guess my switch to a low-carb diet was very abrupt and it seems like I put too much stress on my body during the last year. I am now trying to reverse that with more carbs and better sleep.
Hi, I started low carb in Jan 2013 and have been losing weight (a lot at first and now about five pounds a month). A few months ago I started having these symptoms (of feeling extremely cold and muscle fatigue, losing hair, etc). I started taking magnesium/supplements and made sure I was eating enough fats and calories since I really reduced them – though not on purpose. This seemed to make things better and I would have days with bursts of energy. Now a few months later it is happening again though I have not slacked off in making sure I am eating enough. I recently was reading about certain things (PUFAS, etc) being stored in your fat and as you are losing weight that these may be being released into your system. Have you heard anything like that, I am a relatively new follower of your blog/Facebook, so forgive me if you have addressed something similar already. Do you think it is possible that these work themselves out the longer you remain low carb/Paleo?
Hi! I recently had my cholesterol levels tested, and the doctor said my HDL was too high, at 63. But i read your book, Deep Nutrition, and i was under the impression that was good. But then my triglycerides were 49. is that really low? there are resting levels….
On another question, do you recommend any holistic doctors in NYC or Chicago?
Thanks!
I believe you probably mean fasting levels not resting levels.
There is no such thing as HDL that is too high. Triglycerides 49 are fine.
See the list of low carb doctors at the bottom of this post https://drcate.com/make-an-appointment-with-dr-cate/
Thanks so much for the prompt response!!! i only wish my doctor here knew what she was talking about 🙁
I live in England and have recently started the Terriann 123 plan. It is a zero carb diet for 10 days and then introduce healthy carbs after. I am hypothyroid and whilst losing weight on this plan am now concerned it could cause me more problems in the long run? I am on 175mg of Levo and feel tired and lethargic all the time even off plan.
Try going gradually instead. These ten steps have helped my patients and of course there are plenty of questions answered in our books.
I had the opposite effect – after going low carb, my thyroid went into the stratosphere, with T3 and T4 levels being 3 times higher than ‘normal’ and my specialist expecting me to go into a thyroid storm. I did not associate it with the diet, but decided to leave the diet go until my thyroid was under control. Could it have had something to do with the low-carb diet?
I just had the Gastric Sleeve surgery two weeks ago. I am forced into low carb because Imof how little I am eating, and what I am allowed to eat. I am now on puréed foods. I am getting around a little over 30 grams of carbs a day. I cannot do this gradually. I already am being treated for a hypothyroid. I don’t know what to do. My whole body itches. I am supposed to see my doctor, but they don’t seem to have heard of problems in Ketosis. Is there other help besides doing low carb gradually?
There are many potential explanations for your symptoms aside from thyroid, each with their own unique solutions. It’s best to get help from a low-carb professional in your area. I have a collection of links under the “About Dr Cate/Make an appointment” tab, at the bottom of the page
I jumped into the low carb diet because in the past I had been able to lose weight easily on it. However this time there had been heart issues in between having to have two stints , I had been eating lots of carbs and sugars etc and Hashimoto had been diagnosed. After about 3 weeks I noticed a lot of fatigue but more importantly my heart rate slowed to a low of 57 resting and not going up much hight during the day. Could the low carb diet cause such as this? I introduced oatmeal back into my breakfast and had some rice last night with my dinner without noticing any change. How should I proceed I do need to lose about 40 pounds according to my DR.
[…] across this fantastic article that pretty much confirms my the conclusions I came to after my recent thyroid tests, only she says […]
[…] http://delaineross.blogspot.com/2012/04/paleo-diet-not-just-for-fat-loss.html https://drcate.com/going-low-carb-too-fast-may-trigger-thyroid-troubles-and-hormone-imbalance/ […]
I was low carb for a year. less than 50 a day. i felt amazing, AMAZING. however, when i went off the diet, my hormones went insane. my periods have been all over the board, the doctors diagnosed me as perimenopause and I began losing hair on my head, growing hair on my face, insane acne, ( i just turned 30 ) my psoriasis has spread from a 3 cm patch that i have always had, to all over my scalp. my skin is extremely dry, I have horrible pms. anxiety,depression, cold all the time, cramping hands.all after stopping low carb. these symptoms came on within a week of eating normal again.My doctor advises me NOT going low carb again, i have been eating healthy and excercising, no more than 1400 cal a day, and i have slowly gained 40 pounds. what do i do??!! i want to go lc again but doc says no it will make things worse
Could it be candida? Maybe try a diet more like perfecthealthdiet.com or candidaplan.com?
[…] https://drcate.com/going-low-carb-too-fast-may-trigger-thyroid-troubles-and-hormone-imbalance/ http://earthydigsohiostoneage-today.blogspot.com/2012/09/click-these-points-of-interest.html […]
[…] rest. Moreover, you might try to specifically add in some slightly starchier allowed foods to help ease you into the transition, such as sweet potatoes, parsnips, and rutabagas. This is especially important if you have an […]
Hi,
I am a 37 yr old male weighing about 220lbs.I recently started this diet (low to zero carb).I have been doing this for about 2 weeks now and my ldl level has shot up to 220+.Triglycerides are very low (about 75) and the HDL numbers are low too (36).Total cholestrol is 274.The CRP test that measures that inflammation came out negative (0.8).Still awaiting the results of VAP tests.
Can just 2weeks of zero (low) cab diet cause this?.I dont have any familial history of cholestrol.I am thinking of now reverting back to my normal (high carb) diet for a month and get my cholestrol tests done again to see if it become normal.I am thoroughly confused.
Can you provide any recommendations if I should continue with the low carb diet or revert back to my old diet and start again by slowly cutting down on carbs?.Should i wait some more time in this low carb diet and see if it makes a difference or am I going down the wrong path?
I was doing great on my low carb woe for about 10 months. The problems started when I tried to go VLC to break a long plateau. Within 3 days I had a terrible anxiety attack (I’ve never had one before and didn’t even know what was happening). I immediately went back to eating normal low carb and never really felt “right” again. After several weeks I tried again to lower the carbs and all heck broke lose. Anxiety went through the roof and I couldn’t sleep (can’t fall asleep/can’t stay asleep). I increased carbs 3 days ago and still haven’t regained sleep. I had one night where I didn’t sleep at all. The other nights I slept but not long and not well. I’m left mystified. So many say that carbs are completely unnecessary for human survival but if that is true why does reducing them so far make me feel so terrible? I don’t think I transitioned too quickly. I gave up sugar first then I went to about 100 gr/day then lowered further to around <50 gr/day. It's only when I attempted <20 gr/day all these problems started. I have an appointment tomorrow with a low carb friendly naturopath to begin the process of evaluating my thyroid, cortisol and other hormones. This whole mess is truly upsetting.
After following advice from Paul Jaminet to add back some starch to my diet (according to him my symptoms were classic glucose deficiency) I am starting to bounce back. I am sleeping better and feeling less “ill” overall. I have a ways to go to feel optimal again but so far I’m thrilled to be turning this situation around. Time will tell what adding these “safe starches” will do but for now I’m thrilled to be sleeping.
Thank you for the great information. I’ve been yo-yo dieting over the last thirty years. Up to the age of 21 I was a serious athlete and now, am mostly inactive due to work schedule etc. I go to an ND and am treating my adrenal fatigue and am at the beginning stages of insulin resistance. A few years ago, in 2009, I lost fifty pounds going low carb, low calorie on Lindora but hit the wall with the symptoms you describe in this article and the last few years have gained all the weight back and am on T3 supplementation. I’m so confused about the best approach towards nutrition and wondered if you can recommend someone who can help with dietary changes in Orange County Southern California area. I’m currently a few days into a sugar cleanse, incorporating green smoothies, bone broth etc. and I’ve managed to gain a pound. I’m currently approximately 75 pounds overweight. Thanks for any help you can give!
Links for you
http://paleophysiciansnetwork.com/
http://lowcarbdoctors.blogspot.com/
http://primaldocs.com/
[…] same symptoms as severe thyroid hormone deficiency. This excellent article by Dr Cate explains how going very low carb can trigger thyroid troubles in more […]
I have been doing low carb for a couple of years. I found my A1C to be 5.9 about 2 yrs ago and I became very strict. It’s down to 5.5 and I’m still striving to lower it. The problem lies in my latest thyroid tests. I feel fine, I workout, I’m 114 lbs at 5’3″. I’m 58 and have been weight training for almost 30 yrs. I walk every evening, and I do Peak 8 cardio 2x a week. My last TSH was 5.08, T-antibodies 7 and <20, Free T4 1.11, Free T3 2.1. I have no fatigue or any glaring hypo symptoms. My AM temps tend to be lowish (97.3-97.7). My question is …would it be safe to take herbs like Ashwaghanda and Guggul and the iodine that Byron Richards prescribes on his site http://www.wellnessresources.com? I am not comfortable messing around with hormones.
Please help me understand this paleo/high cholesterol/hypothyroidism delimma. I have eaten Paleo on and off for about a year – recently did the Whole 30 Paleo version. I lost 5.5 pounds, 4 inches off my waist, with a total of 9 inches overall. At the end of it, just so happened it was time for some blood work to be drawn for wellness insurance benefits plan and my cholesterol skyrocketed and now I have been diagnosed with hypothyroidsim. CHOL 135 to 412; TRIG 59 to 221; LDL 86 to 292; HDL 50 to 76 / and they said my Thyroid testing was over 100, norm should be .45 – 6.675. I am freaking out. I thought this was a healthy plan for me. I have felt really good. Felt stronger than ever. Started Crossfit over 10 weeks ago and felt like I was stronger than I had been in a long time. I am a 49 year old female. So confused now as to what I should do. I do not want to take medications if I do not have to.
Karen if these labs were not done fasting the lipid numbers are not meaningful. If they were, you may be doing a little too much fruit or carb or have the wrong oils. Best bet is to find a nutrition-literate practitioner. For a listing check these sites: http://primaldocs.com/ and http://lowcarbdoctors.blogspot.com/ and http://robbwolf.com/2011/02/08/paleo-physician-network-is-live/ or schedule a consult with myself https://drcate.com/make-an-appointment-with-dr-cate/
Hi Dr Cate
As with most topics in health the arguments go back and forth regarding the subject of lo carb diet and thyroid. I find that with my patients T3 reduces and T4 increases due to the inhibition of T4 to T3 conversion. That finding, in part, supports the current data.
However, not all patients respond the same to that decrease in T3 and that, of course, reflects the complex relationships of the body and the biological individuality of the patients.
Interestingly, alcoholics have a faster conversion of T4 to T3 and therefore the Lo carb shift to T4 may be an unexpected treatment for them (or hindrance). Although, it is still too early to tell.
Good luck with your patients.
Dr Downing
Director of Clinical Education & Research European Council of Diplomat Doctors
I went through this phase. It is called the “Keto Flu”. It is entirely normal and passes in a week or two if you are managing your macronutrient ratio and electrolytes effectively.
It’s hard to stay on a low carb diet when you are doing many sports.
I don’t think that can be the case – after all, then the low carb wouldn’t make sense, because you’d be burning less because you’d be sedentary.
Hi.
I was wondering if this kind of a diet/ exercise plan will work for fat loss without muscle loss when I am a 78kg, 184cm male in my early 20’s:
Monday: HIIT (20 min) – 2200 kcal
Tuesday: Heavy upperb. – 2450 kcal
Wednesday: Free – 2200 kcal
Thursday: Heavy lowerb. – 2450 kcal
Friday: Free – 2200 kcal
Saturday: Mixed calisthetics – 2350 kcal
Sunday: 45 min steady cardio – 2350 kcal
where
2200 kcal = 200g prot, 120 g fat, 85 g carbs (veggies)
2350 kcal = 215g prot, 130 g fat, 85 g carbs (veggies)
2450 kcal = 240g prot, 105 g fat, 135 g carb (veggies and fruit)
and a re-feed of 3000 kcal every 14 days with the heavy lifting on thursday looking like this:
240g prot, 138g fat, 200g carb
Thanks a bunch.
p.s. I also take 600mg phospatidyl serine, 400 mg EGCg, multivitamin x2, 5000 IU d-vitamin and will start taking 10g l-leucine on workout days (5g on non workout days).
That looks pretty great. Though you didn’t specify your 200g carb day I’m guessing it too comes from fruits, not junk.
just found you and this thread… exactly what happens to me!!! i purchased and read your food rules, hoping it would answer this question but it didn’t. just wondering how high my carbs should be to start and how quickly i can lower them.
wow- excellent.. that article explains this issue so well….
If only i wasnt diabetic so I could try carb cycling and also perhaps adding back more carbs to then reduce them gradually – but the irony is that I wouldnt have ever been interested in low carbing unless I became a diabetic in the 1st place ! lol
some days I have an extra meal meaning I get to 40 or 45 grams carbo per day. but not often….. when i initially went low carb back in April 2010 I adjusted very easily – but my LDL cholesterol went from 80 to 285!!!! – now finally with T3 its reduced back down to 159 and prob still on its way down further..
Needing to take thyriod meds (t3) for the rest of my life is worth it to be able to stay on low carbing to get good blood sugars right?… (I have diagnosed Hashimotos and type 1 diabetes)….
I think this topic needs to be really put out there as much as possible so people going low carb may be able to avoid these problems or be prepared for them…. If I had of known this 2 years ago then it would have saved me many headaches wondering why my LDL suddenly ski rocketed.
Great Post Dr Cate…….loved it, i went from sugar burner to fat burner overnight and only had about a week of feeling like shit…now a pure fat burner with no side effects luckily 🙂
Hi Dr Cate,
Your post makes complete sense to the way I’m feeling, but I wondered if you could fit some more symptoms into your hibernation theory. I think they fit but I’m not sure how. I’m 40 now, not overweight, but have had very low energy levels and hair loss for a few years. Insulin resistance was mentioned, but nothing further was said or done. My thyroid levels were nearly normal, but I was prescribe synthroid. This made me worse. I was prescribed Armour instead and this made me worse too. I’ve been gluten and dairy free for ten years and processed food and sugar free for 5. I gave up all grains about a year ago and ate lots of fresh organic produce, sprouted food, meat on the bone and broths, but no fermented food. Three months ago I started a very low carb candida diet. But just before I started it I had been prescribed a low dose of T3. This also made me feel terrible, with no energy and a longing to hibernate I felt like a leaden zombie. So that was stopped. I’m still on the VLC diet, but still feel awful. I’ve tried dessicated adrenal (containing small amounts of adrenal hormones) and cortisol on it’s own. These have the same debilitating effect. And so does Vitamin D (a summertime sunshine vitamin) and even coconut oil (a fat metaboliser). Since starting the VLC diet I have got fatter and flabbier, but my hair loss has slowed right down. Also I feel at my worst just after eating and it doesn’t matter what I eat but a bit brighter if I don’t eat for a really long time. However when I do that I feel even worse the next day.
Can you explain why thyroid hormones, cortisol, vitamin D, and coconut oil (and eating!)make my symptoms worse, and why I’ve got fatter on the VLC diet, using the hibernation theory?
I’m scared to eat carbs again and don’t know which ones to try first.. The candida diet recommends beans/pulses. What do you suggest?
I am a 6 yr survivor of Thyroid cancer. I had to have my thyroid totally removed. I take 150 mcg Synthroid daily. Been on the Paleo diet for 5 days now…..have no energy at all, getting cranky and moody. I feel like I do when I have to come off my Synthroid for 6 wks to have a cancer scan done….HORRIBLE, a real Nightmare.
Is this diet going to work for me?? Should I even be trying this type of diet, not having a thyroid?? I am truly at my wits end…..I am approx 100 pds over weight and have not had real energy in years.
Can anyone shed any light on this for me??
Hi Dr. Cate, great post. I started eating lower carb in late February of this year and then in March cut out all grains/most starches. I’ve lost 35 pounds so far and hope to lose another 40 – 50. In June I noticed my hair was thinning but thought it was my imagination until my husband exclaimed, “you really are thinning” one day. Ugh … I have had some dry patches of skin on my face but no where else and I don’t think I’m fatigued (I have two small kids so hard to say … lol). I did a search a few weeks ago and read what Dr. Eades says about telogen effluvium and assumed that maybe it. How can I tell if it’s that or a thyroid problem? I feel so much better eating this way but this situation is a little distressing. Thank you!
This is exactly what happened to me. After being on Atkins for 4 months I lost 47 pounds and felt great at first. Then the fatigue started, the dry skin, and worse of all my hair is falling out like crazy. My thyroid tested normal. Please, are you saying that by adding back carbs (say maybe fruits) I can stop these symptoms? I really don’t want to go back to eating bread and sugar.
Possibly. Atkins is not necessarily a balanced diet (several of the Four Pillars are missing) and until you identify and add back what you are missing it may be easier for your metabolism to get a break from ketosis for one to two days per week using fruits, sprouted grains, beans–whatever suits you best.
Hi,
First, I want to thank you for your book, Deep Nutrition. I found that it explains very logically some mechanisms in the body that “regular” doctors simply dismiss as explainable.
I say this due to the experiences of my parents which have several health issues but got virtually no useful advices beside lots of pills and a recommendation for bypass.
I finally convinced my mother to start using Kefir and she was ecstatic to have her fasting glicemia drop from 237 to 125 in few days.
I for one had as a teenager aches in my joints following a streptococcal infection. That lasted for over a decade when I quit eating meat. Even now, my joints are completely free of aches, except low back pains due of a spina bifida occulta. Now, at 40, my joints are a bit stiff and I annually „clean” those using bay leaves infusion.
While I was vegan, I had little interest in eating healthy, so after sever years I discovered a severe anemia. It got better with medication. So I went back on meat, liver, but anemia kept coming back.
After having my second child, I gained a lot of weight I could not loose for vanity purposes.
For about a year, I decided to get back my health. I hate taking medication and it seemed with my family history and borderline obese I wasn’t to far away from it.
I found the nourishedkitchen blog which opened up a window to new possibilities, introduced me to bone broths, sprouted and fermented foods, W.A. Price studies, your book and lots of interesting stuff.
So I cleansed my urinary system with lots of cinnamon and of stones with the parsley tea recommended by Dr. J Howenstine.
I had a gallbladder cleanse with Epsom salts, olive oil and lemon juice, which got me clean of the bitter taste in my mouth and the dull pan in my liver. Plus I have sub-lingual bleeds every 6 months (ancient custom here, in Romania).
My digestion improved a lot with Kombucha over only two months. I also started to take Kefir which is clearly great to put on my skin instead of night cream.
So I make efforts to clean up essential systems that are meat to maintain health, systems that after years of imbalanced lifestyle are overwhelmed and in need of assistance.
I also take fish oil, alpha lipoic acid, and chromium, mostly for pancreas.
After only a few days on Montignac, I went to Atkins, about a month ago. The rapid weight loss was, of course a lot of water, which made me very dizzy, but went away as I learned to drink water with lemon and have a pinch of salt afterwards.
But after about a week on Atkins I had a horrible day, I felt like I was as dry as a desert inside, I felt like a something was crushing me from inside, despite drinking plenty water. So I went to my kitchen and had a huge glass of celery and cucumber juice (now wanting to make something out of sweet fruits).
Therefore, I decided I need to eat more raw vegetables and fruits than only two tomatoes and a dozen of olives.
And since is the time of year for strawberries and raspberries I eat them, more that what is “right” for a low carb diet. Most of them I let them ferment overnight in Kombucha (thanks to your passage about monkeys and the way they digest fruits). I hope that will lower the sugar content, while keeping the enzymes alive. I love the taste.
I found out that adding grains (as in homemade noodles) is not the best thing for me, as I feel the post-eating fatigue if I ear more than a few bites.
I also saw some information about alkaline diet, which makes sense to me.
Thing is in low carb, ketogenic diets is easy to eat lots of proteins like lean meat that will have a certain impact over the body, acidifying it. I think that it also makes sense to eat according to seasons, eating most what is really fresh in the local market. I doubt cavemen hunted and eat a mammoth every week all over the year.
And food is more than nutrients, the more energy of life which translates in physics as enzymes and so on, the more energy you get in.
When starting to loose weight and gain health there are massive doses of toxins released from deep within our tissues, which may make us feel worse before we get better.
Thank you.
I have been on the Paleo Diet for about a month. I am thin for my height, not on this diet to loose weight. My husband read something that indicated it could resolve stomach acid problems so I decided to give it a try. Also, I have Grave’s Disease (hyperthyroid). I have read in a few places online now, including this site, about the issues with people who have hypothyroid, but not hyperthyroid. I have been on medication for this for over a year, and the only time I have had a recurrence of symptoms was when getting off the medication for a week, and now with this diet. Since being on the Paleo Diet my symptoms are unbearable: extreme anxiety, shakiness, no energy, can’t sleep, feel like I’m going to pass out all the time, cry all the time. I suspect it’s this diet and something similar to what you discuss on this site for those with hypothyroid. Have you run into anyone else who has hyperthyroid with these symptoms when on Paleo Diet? I went cold turkey, by the way. One day eating carbs, next day not.
How many days/weeks into Paleo did you begin noticing these symptoms?
I had some symptoms immediately, but the websites all said the shakiness and light headed feelings were normal and to give it a few weeks, so I did. The anxiety and sleep issues hit around 2 1/2 weeks and are getting progressively worse.
I’m assuming someone is checking your glucose levels and your only endocrine (hormone) issue is hyperthyroidism. You may have had some insulin resistance even with normal weight and one less-than-ideal but easy way to tell is if your glucose is over 90 in the morning after an 8-12 hour (and no longer) period of fasting. If this is the case you simply need to proceed more gradually with the diet changes. Even if you do not have insulin resistant gradual change is prudent. The changes you made in adapting paleo likely involve not only cutting carbs but also increasing protein. These beneficial changes demand upregulation of many genes that your previous diet may have downregulated and this makes gradual changes a necessity. (If this information has been helpful, please SHARE this post everywhere! 🙂
Thank you for this article. After 8 months of very low carb dieting I hit a plateau, and had a bunch of symptoms: cold hands, constipation, dark circles under my eyes. All hypothyroid symptoms.
Having lost over 100lb in a year I am terrified of eating carbs again, but I’ve had to do so. I’d still like to lose another 20lb, but it’s not happening. Frustrated, and worried about my poor thyroid!
Great work on the 100 lbs! That is fantastic. There are so many reasons you may be hitting a wall here and permanent carb increase is not necessary the solution. I think you may neet to get some help from a good low carb doctor. Check out the American Society of Bariatric Physicians website, or Jimmy Moore’s website.
I have shifted from high protein via meat, no milk/eggs, relatively low carbs (no wheat, corn, potatoes, minimal sugar) to your approach – adding in raw whole pastured milk products (yogurt, cream, milk, kefir, cheese, eggs). I did not need to lose weight but needed to reduce inflammation (asthma, osteoarthritis). Since starting, have lost 7 lbs- from 125 to 118 (I’m 5’6″) in about 6 wks. Should I be concerned? Should I change something? Should we talk?
Good for you for making healthy additions. I hope you are also feeling better. If not, feel free to contact me about a consultation (click on tab: make an apt).
Oh, and I realize I should eat protein as well as fat with all meals but the point I wad making was that before I could eat 50g sugar + carbs in a sitting, and yes I’d feel.the crash afterwards.and would sometimes feel hypoglycemic, but two weeks later and I have a much worse reaction to 1 cup of veggies – There’s got to be worsening insulin resistance happening by cutting so fast.
Rachel, I will be doing a post soon about this common issue that is very often misunderstood. Stay tuned by subscribing and please pass the word around if it’s useful to you because this is the NUMBER ONE problem with folks going low carb on their own, that is, without medical guidance. Meanwhile, I recommend you call around to find a low-carb or Paleo doctor in your area.
I’m wondering if I should keep on truckin’ through the hard times until my body adapts or if I should slowly incorporate a few more carbs per day? I feel like just reverting to my old diet would be too drastic for me again, seeing as how a cup of steamed greens caused such a huge dip in my blood sugar.
Any advice would be cherished.
And by low carb I mean from cakes, toast, pastas to one piece of toast and/or bowl of oatmeal with almond milk a day. Drastic. It’s only been a week and I feel so much more insulin resistant now than before and have been searching for WHY because I’m now eating no carbs other than veggies.
I’ve had 3 episodes of hypoglycemia ~60 blood glucose level with symptoms in one week. I cant eat a bowl of veggies with avocado without getting hypoglycemic.
I’m 24 and thin but for 3 years I’ve had anxiety, adrenaline rushes at night preventing sleep, feeling hungry all the time. I was told it was in my head and given anxiety meds. Truth be told, I never took the meds. I wasn’t convinced. I’ve been cutting so many different “allergens” from my diet attempting to find a “culprit” and after being diagnosed with PCOS recently, I realized my long list of symptoms sounded like insulin resistance!
So without medical guidance I went low carb.
Susan,
Oh, I can really feel the frustration, and I understand it. For a lot of us, the books—even when we’ve taken the time to carefully read and study a number of them, as you have—can only take us so far. I’m so glad you commented, because I promise you there are a great number of others who have hit the same kinds of roadblocks.
It for people like you that I decided to set up a one-on-one consultation service. Often, people have, all by themselves, managed to get just about everything in place, but cannot get those last pieces of the puzzle in place. That’s why I recommend that, if at all possible, you engage in a one-on-one consultation with a health care professional familiar with the fundamental concepts laid out in Deep Nutrition.
If you think you might like to set up an on-line consultation, click here to learn more.
sorry , i meant should i go for a high carb diet flush out RT3 and then slowly start on low carb ? not sure what to do..Been trying lots of diets and exercise but not able to loose weight.even if i loose it comes back again.Very low carb i feel nervous and not able to function.but what i have seen is if i keep my excercise constant i loose weight.But i dont have energy most of the days to workout and skip workouts.Please suggest what should be my next step.Thanks a lot
so low dosage, plus low carb crashed me.i knew low carb is the way to go , but was not sure why i crashed.Now everything makes sense to me.and always i have had pretty high insulin levels and hypoglycemia.and its a vicious circle.Not sure how to break it.I did my blood work.TSH- 2.12 , Free T4 1.61 (0.82-1.77) , Free T3 3.0 ( 2.0 -4.4 ) , RT3 43.2 ( 13.5- 34.2)
Is my RT3 in a very bad shape.Do you think if i should go on a low carb diet with this RT3.So should i go for a high carb diet
Hi Dr Kate ,
I am have hypothyroid for the past 12 years and i have been on Levoxyl.i am nealry 100 pounds overweight.I tried Tim ferris diet ( low carb ) for 20 days.I felt great in the beginning , but crashed at the end of 20 days.I was bed ridden for almost a month with low BP , dizziness and severe hair fall.My bad timing , i started birth control pills 2 months before starting the diet and was feeling hyper.So my gynec by mistake asked me to reduce the thyroid tablets.
Hi, Dr. Cate!
I read your post and now wonder if I, indeed, DID cause my pituitary or thyroid to tank. After being a vegetarian/vegan for all my adult life, I ate Paleo/Primal after the birth of my child and lost all my baby weight. I was later put on thyroid meds and sex hormones and have gained all the weight back and THEN some. Still gaining. I eat moderate carb and wonder if I have to increase the carbs more or wait till I get the meds correct. Is it even possible to lose when hypo?
Whey hypothyroid is treated you can lose weight. Many women develop thyroid problems after delivery and it’s unclear why, but of course I suspect a pro-inflammatory diet has something to do with it. As far as what you should do now, I think you may benefit from working with a low-carb doctor in your area. (Or you could book an online consultation w/ me!)
Thank you, Dr. Cate! I really could use a consult with you and will save to do so (as I’m getting nowhere with the professionals I deal with now). Thanks again for your reply.
searched ‘sleep problems’ and this is the closest that came up, I am having problems waking up in the night hungry. What’s odd is that I felt full and slightly bloated after dinner (sashimi and beef w veg) but now I’m hungry. I’ve tried adding in extra fat (butter and lard) but it doesn’t seem to be helping. Thanks for any suggestions, I’m 37, lean and active and with no obvious health problems that might be the cause.
There are numerous potenial causes underlying sleep disorders so giving you advice without a complete history could certainly send you down the wrong path as well as miss something important.
ok, thanks for the reply. I live in Japan (Okinawa, of all places!) so open-minded healthcare can be hard to find – I once went to a doctor and all I got was sleeping pills 🙁 I’ll consider a consultation with you but in the meantime are there any books you can recommend that might help? Lastly, still couldn’t sleep last night after eating low carb, so I got up again and had a banana, and was then able to sleep. Could carbs/blood sugar be the issue? Thanks again.
I’ll add that I don’t think it is stress. I’ve done a lot of this: http://www.focusingresources.com/index.html (I cannot recommend this highly enough!!) and am now feeling happier, more in control, and more able to enjoy life than I have in years. It does feel like diet is the issue. Thanks again.
Quite possibly but there are numerous other explanations that a history might uncover if you get to a good doctor!
ok, thanks again for the replies (I’m sure you are very busy)! If adding in a few more carbs doesn’t solve the issue then I’ll look into the issue further, maybe get some bloodwork done (maybe even consider a phone consultation with you). Thanks also for your books, I’m looking foward to the TRIM book when it comes out.
Without knowing background information that is not appropriate to discuss in the context of a blog I can tell you that I have yet to see a patient with abnormal thyroid function tell me they feel good! But–one can have normal function with abnormal growth processes so the ultrasound is important.
Hi Dr. cate!
Ironically, I went for an ultra sound today of my thyroid. I do not have results but my doctor wanted to be safe since she felt the swelling of my thyroid. I recently switched drastically from high carb to low-carb high fat. I’ve been successful and have not felt any symptoms from hypo/hyperthyroidism. I exercise 3-4 days a week for about 1 hour. Running or weight lifting and usually eat 3 meals a day.Should I incorporate a little more carb intake? Or will this go away? I feel great
Hi Dr. Cate. Would you suspect something similar with hibernation mode for long term low carbers too? I’ve been low carbing for many years and have lost 175 lbs, but have hit a long plateau of over 4 months now with 30 lbs still to lose. My TSH has been in range with levoxyl (checked regularly the entire way), perhaps I should get my reverse T3 checked? I don’t have any symptoms of fatigue, etc. and my daily carbs is around 40 or so (30 net carbs) of good veggies, lots of fat calories, etc
Unlikely to be a thyroid issue without the expected symptoms. You’ve lost an amazing amount of weight, very impressive, and with only 30 to go for a normal BMI then it’s probably just an issue of your body needing to be “sure” you want it to keep going. There’s a lot going on at the cellular level that requires consistent ‘messaging’ in the form of nutrients, sleep, exercise. Keep up the good work!
Thanks! I may ask my endo to do the reverse T3 test the next time just to see. But overall, I feel pretty good and love the way I eat. I’m use to plateaus but this is the longest yet so I’m looking for ideas that might help me get past this one. I’ve tried adjusting nutrients (upped the fat and calories, eliminated stallers like dairy and yeast foods) and may trying upping the carbs next to see if that helps. Sleep and exercise are solid too. Started on bone broth this week too. Thx!
Also, one more thing. What do you guys thing on this food combining idea? That one should not mix protein with carbs because the digestive juices cancel or whatever. I been doing that but I really don’t find much support for it and it does not make sense. For, example, Weston Price showed how primitive people eat their protein combined with carbs, almost al the time. And they were pretty healthy.
I was on a low carb diet for a about a year (<100 g) but I could not gain too much muscle with it. I am a fairly slender guy, and upon adding high glycemic carbs and protein after a workout (raw skim milk with banana, some grass-fed whey protein, a tbsp maple syrup, no fat) adding muscle has been easier and I feel more energetic. I eat about 50 grams of carbs post workout to induce an insulin response. I still eat high fat the rest of the day, just not around my workout. Any thoughts?
It’s an interesting idea, however in reality I’m sure how much insulin your body needs to ‘sop up’ those 50gm of carbs after a workout b/c hungry muscles will do this in the absence of insulin. You’ll probably get a better response by doing workouts in the AM, eating a big meal, then taking a nap.
I do workout in the mornings and always eat after that. Before I used to have a smoothie with raw whole milk (or coconut milk) and 2 or 3 eggs and it was sort of hard for me to gain muscle. But now I can see that I am gaining more lean mass after getting the carb/protein combo and also have more energy. I guess it’s still okay since I eat less than 100 carbs a day. What do you think? By the way I love your book Deep Nutrition; it got me into bone broths! Thanks Dr. Cate!
Carlos, perhaps you might find interesting the Cyclical Ketogenic Diet. It is designed for body builders. Consist of alternating low carb, for let’s say 2 weeks and a few days of high carb, to replenish live and muscle glycogen and gain mass. I saw it in Lyle McDonald’s book Ketogenic Died. Also there lots of information for sport oriented peoples. If could send it by email if interested.
Thanks for guiding me here Dr. Cate,
I get it, so adapting to low carb is key to maintaining t3. I also wonder what you think is true for athletes who expend more energy, if they may require more grams of carbs, with increased overall expenditure?
Also, do you think that taking t4 supplementation may result in more thyronamines if rt3 mechanisms are in place?
Also looking forward to a phone consult, as I was coming to see you last week, but the drive is simply to far.
Kindly,
Bevin
Athletes do require more energy, but I do not think it would matter whether it comes from fat or glucose. Those athletes who are able to store more muscle glycogen would tolerate a higher glucose intake. And yes, to your question about t4 supplementation.
Thank you for the article! I went Paleo very abruptly and have had the hibernation fatigue and hair loss, and also a slew of severe PMS-like symptoms like irritability and depression. I hope the gradual approach will help.
Cool post Dr. Cate, maybe if you have a chance to work with someone that has had this happen to them and your able to coach them through it you could post about how you were able to help them. I know you can’t really give medical advice but to know it’s possible to transition over slower would be encouraging. I’m not really willing to go back to low carb because of the anxiety and everything else along with it, even after working with a practitioner that says “it works for everyone”.
Another trap you can fall into. You cut wheat and sugar, but you don’t have a lot of meat and cheese. Your body gets into a very alkaline state. You feel miserable. You wonder why your heartrate spikes when you take a vitamin c pill or 1/4 tsp of rice syrup. You eat more acidic foods like meat, cheese, and black tea and you feel like king of the world. And by you I mean me. No one talks about this except a local dr I know.
This is fascinating. Ive spent 2 years looking for info on “when paleo goes wrong.” I started paleo 2 yrs ago. Felt awesome. 3 weeks in, massive gallbladder attack. Fought my Gb, and these thyroid symptoms, for 18 months. Finally had the Gb out when I couldn’t tolerate the pain anymore. Now I’m working with a traditional foods nutritionist to get back in the game and resolve my prediabetes. Im resolving to not do Lazy Paleo, relying only on meat and nuts! Dark green veggies with every meal…
I’m still on my quest to deal with Very Challenging Symptoms…and am mostly coming up with more questions than answers! But it’s fascinating! And I just listened to a podcast interview with Chris Kresser last night, and took some detailed notes because I thought others might appreciate his thoughts on thyroid and hormonal health: http://www.lifeisapalindrome.com/updates/some-fascinating-facts-about-thyroids . His approach complements yours, Dr. Cate–thanks for continuing the discussion.
-Sara
Sara,
Thanks for sharing, very informative stuff!
Awesome article Dr. Cate!
I was excited to learn I am not the only one interested in the effects of hibernation. I’ve long thought it was so fascinating. Bears go to sleep in early Winter, wake up several months later with almost no muscle loss, tons of fat loss, little movement during the winter, they stay normal thermic, yet their HR plummets and they don’t even really drink water. Amazing.
Thanks!
Mike T Nelson PhD(c)
You are so right, Margarete. I sought the aid of a doc for hypertension. He gave me a prescription which lowered it to 140/80. I was not happy with this but was told it was okay at my age. Saw an endocrinologist to get hormones checked, told him about zero libido in addition to other stuff. He told me it was normal at my age. It’s wrong to tell people in their 60s they are old. I have contacted Chris Kresser & plan to see Dr. Cate (calling later today)
Both are about 45 min from me!!!
Lucky you to be near them! Good luck!
My doctor will tell me to take Prevacid or some other medication, I don’t trust medication…I do, however take my thyroid med daily. I refuse to take statins, too, they make me feel like crap. therefore I am trying to live a healthy life instead and eat well.
so, that’s why I think people will try to make these changes on their own, fearful that a doctor will either ridicule them or just prescribe some other medication or both!
Good advice. : ) One more question: if a woman had Hashimoto’s thyroiditis, is it caused by being low carb or would being low carb along with thyroid meds actually help that condition?
Thank you. Dr. Kresser is the reason I first tested my blood sugar and found it high. I’ll contact him.
Best of luck and tell Chris Dr Cate sent ‘ya.
Should he be trusted? He states that the paleo premise that “carbs spike insulin which causes insulin resistance” isn’t a fact. http://180degreehealth.com/2012/02/12-paleo-myths Would one with PCOS be best off eating a healthy diet (four pillars) with no veg. oil, packaged foods, sugar, etc. while staying on grains? All the medical attention that is required b/c of these “programs” are expensive not to mention all the food and supplements to help the conditions that result after the diet.
Kristen
While it’s important to read and learn online I find that sometimes one needs professional guidance to avoid feeling lost. Matt Stone is just one of the people out there saying low carb is dangerous, and there will be other people who say the opposite of everything else that I say. To really get to the root of your trouble, we need to get a more complete background including blood tests, family history and more, which I look forward to doing during a phone consultation. That will give me an opportunity to better advise you and give you an opportunity to decide if what I say makes sense to you. For now, rest assured that you are eating better than before, much better from the sound of it, and that is always a good thing.
Wow. When I read Matt Stone’s description in his Diet Recovery Book, it’s like he’s talking about me. This is the first diet I’ve ever done. Five months later, I have worse symptoms than ever. I did it to bring down my glucose levels. That worked but everything else seems to be falling apart. When my husband read Matt’s description, he said, “For the love of God, please read that book.” Ouch. I must be meaner than even I thought. : ) So what’s the verdict? Is he on to something?
Hi Dr. Cate,
You describe my symptoms perfectly! (Except my insomnia.) My rT3 is at the top of the normal range, else normal. Also my serum ferritin is below normal, am prediabetic and cortisol is high in the morning only. I’ve started iron supplements and considering Thyro-Gold. I’m scared to abandon the Leptin Rx (J. Kruse) I’ve been doing for 4 weeks. Any hand-holding/specific advice you can give on how to best reintroduce carbs would be very much appreciated! Thank you thank you thank you
Jill
I’m seeing a theme here of folks getting into trouble with diet changes made on their own.
For anyone serious about making diet changes for their health but has run into trouble doing it on their own, it may be time to seek professional help. Remember, the food you eat informs your genes and has a profound effect on your health, so diet changes are a kind of medical advice. You probably want to get medical advice from people who are highly trained and trustworthy.
I trust Dr Tom Cowan and Chris Kresser, both are available now, and starting in May I am going to be offering online services as well. (see the tab Make an Appointment)
Hi Dr. Cate,
Can you explain why the low carb diet can produce so much gas? since I went gluten free a month ago, I have developed horrible GI symptoms, lots of noise, lots of gas and a mucus in the back of my tongue whenever I eat anything that is not fresh food, even a protein bar or protein shake will send my stomach reeling.
Probiotics may help. I don’t advise protein bars or shakes, for reasons described in Deep Nutrition. Our next book (due this fall) will offer a step by step guide for diet rehab, and in the meantime if you continue to have trouble you may want to consult a professional in your area or online, either myself or Chris Kresser.
Thanks you for a quick reply even on a Sunday! I did start probiotics, but thought that they are adding to my gas issues. I do want to contact you when you offer online services, pls let me know how to do that and how much it will cost! Thank you!
Margarete:
Here’s the info from our Make and Appointment Tab: For those who cannot come to my office, starting in May 2012 I will offer telephone consult between 1 and 3 on Wednesdays and Saturdays. The fee is $175 for 30 mins and $325 for an hour. Payments must be made in advance via paypal. If you would like to reserve a Wed or Sat appointment in advance, please send an email with the date and time you would like to admin@DrCate.com
Currently the first appointment is May 9, the 4-5 slot. Email us with the time you’d like to reserve at admin@drcate.com and when the scheduling function goes live we’ll send you a link. Until then, be well!
Thank you very much!
Dr Cate – I felt encouraged and felt hope finally after reading that you will be offering telephone consults but after seeing what you charge I am frustrated and see that I will be unable to afford it.
The cost of health care is out of reach anymore and for those of us w out insurance and unable to work because of health issues, we are really stuck…will you be offering any kind of sliding scale?
Yes it is sad. Especially as insurance doesn’t pay for doctors to do the counselling on diet changes or nutrition that could help so many people. So right now I am doing only very limited phone consultation. In the future I may get more sophisticated and offer other payment arrangements.
So enjoyed your talk on Paleo Summit, learned much about bone health, supplements, etc. On LDL however, you indicated have never seen LDL fail to go down on low carb. Mine has been going up over 18 months, as it did for others linked in a cholestrol post here. http://perfecthealthdiet.com/?p=4457
My triglycerides are only 20, HDL 85 and have a good NMR lipoprofile, but an LDL of 155 looks bad according to current standard of care. Can thyroid interactions described here cause high LDL longterm?
You offer a perfect example of the pitfalls of focusing on numbers rather than what you are doing an how you feel. The interpretation of numbers changes all the time, and standard of care lags behind actual thought. At a Bariatric society meeting we learned that the most important ratio is Triglyceride divided by HDL.
I think slowly reducing carbs is the way to go. Reducing too fast is very stressful on the body. Your heart rate and blood pressure will rise. I wouldn’t hesitate to have some evil white bread or potato when you feel the adrenalin start to flow. At least it doesn’t have fructose. If it doesn’t feel good, you’re doing it wrong.
Thanks for the reply Dr! Good answer, but left out some details, the frequent urination is something I have had all my life, after persistent bet wetting even when I was 12 years old, I had an extensive medical examination. they could not find any medical cause. thankfully I finally quit bedwetting by setting an alarm around 1 am every night to wake me up to go, after about a year I started waking up normally. I may have to try the pumpkin seeds, how to you prepare them?
I enjoy them raw, but they’re even more tasty when sprouted and lightly salted and health food stores usually carry pumpkin seeds prepared this way.
Hello,
thanks for your explanation, Dr. Cate. I am trying to go paleo slowly, though I am wondering about one thing – I have this “calorie counter” which helps me see how much of carbs, proteins do I eat. But even if I remove all the grains, I still have over 30 g carbs per day. At least. It’s almost impossible to do without them. So how much is low enough? How much do you think is too much?
I advise people to do one meal at a time starting with breakfast. 30-70 gm would be the final goal for all day. Details will be addressed in our next book, which will lay out a program for adapting traditional diets for weight loss and optimal hormone balance.
I’ve tried going at it very slow and just don’t seem to digest it…from what I’ve been reading it seems it’s essential to eat the fats in order to switch from carb burning?
Correct about the need to eat fat w/ protein. This is why Meat on the Bone, meat with all the parts (skin, fat and even bone, see Chapter 7 of Deep Nutrition) is helpful. My next post will allude to this as one of the pitfals of some Paleo programs.
Quick question- any thoughts/reccommendations on how to go low card (something i know i need to do because i CRAVE them relentlessly!) when i dont tolerate fats?? (gallbladder out years ago) ive tried taking ox bile and plant enzymes high in lipase and no help. Tried going primal and added lots of meat/bone broths andn duck fats and ended up in the hospital so sick from the fats! (didnt realize that was the issue until later) Any thoughts??
Thank you so much for your research and time w us!
It’s essential to go slow, ie don’t add too much fat at once. Broth can be skimmed so you remove the fat, if you want to be able to keep that aspect of the diet unchanged.
I tried to eat low fat, high carb diet for years–I ate lots and lots of carbs. Because I have hypoglycemia, I would eat frequent meals with lots of carbs to try to keep my blood sugar from crashing. Then I learned about low carb as a better way for hypoglycemics to eat. At first I felt better and lost 20 pounds. Then, even though I have tried to keep my carb counts to around 20-30 per day, I stopped losing weight for weeks and I feel terrible! like my blood sugar is crashing …
Carol
Good for you for working so hard. You may not be getting enough nutrients/exercise/sleep. Including all four of the Four Pillars of World Cuisine is essential to healing your metabolism, and you may want to work with a bariatric or low carb physician in your area to help with your fatigue.
Hi Dr. I have been low carbing for a few years now, lost excess weight, but I have felt much better and had more energy by eating only 4 pillar food the last 2 months. that seemed to be the final step to rid me of a few symptoms from my other low carb diets, like the zone, and protein power diets, like low energy, and headaches, but one annoying problem that persists is frequent urination. if i am real strict on my eating it actually gets worse, or if I fast. Is there any foods that cure this?
Michael
You definitely want to get your symptoms evaluated by a medical practitioner to make sure there is no infection, inflammation, or other process that may need to be addressed. After that, then I suspect an herbalist or naturopath may be able to make a recommendation for something that would facilitate the production of protective mucus in the bladder. For example, pumpkin seed has been effective for some.
Thanks! I just realized that what I’m going through is thyroid-related in the last month, when I finally did some bloodwork and connected the dots. I started taking pure dehydrated thyroid gland (thyrogold) 3wks ago, and am slowing upping the dose, hoping to see some good.
Sadly, the thyroid & adrenals are some of those nose-to-tail parts I can never get the butcher to return to my farmer when they slaughter the pigs & cows we buy. I’d much rather just eat it than take it as a medicine!
halleluia! you just confirmed an hypothesis i had formed about WHY a hypothyroid like myself can do so well on very-low-carb — thanks! i SUSPECTED that, in the studies that showed low-carbing diminishes thyroid function, the subjects were not well-adapted beforehand!
i did Atkins before i discovered Paleo; by means of a month of very restricted eating and then reintroducing foods, i’ve discovered sensitivities to things i never suspected before. now i feel 20 years younger.
Good for you, keep it up!
This post and Matt Stone’s theories on rebooting one’s metabolism are actually making it all come together for me.
http://180degreehealth.com/2012/01/diet-recovery
Thank you! Pam
Hi Dr. Cate –
This post describes my recent symptoms – but after being low carb for about a year! I seem to have hit a wall – fatigue, dry eyes, low stomach acid, dry skin, low body temperature. I started adding some safe starches but that only helped my eyes. Now I am feasting to raise my body temperature and come out of “hibernation”. I have never felt better eating more starches/grains. I am guessing this is a short term fix until my body temperatures stabilize. This post and Matt Stone’s
… but as an out-of-context state. His theory is very similar to yours, but his solution is not to change to LC or VLC gradually, but to employ cold thermogenesis. His clinical experience & his own n=1 have shown CT reversing disease pathologies & helping avoid the low thyroid problems I’ve experienced (yes, my TSH is low, but my fT3/rT3 ratio is dismal at 7.0).
It’s laid out in his recent (typically cryptic) blogs. Sounds like you’re hitting at the same thing from different angles.
Cold thermogensis affects your metabolism in a similar way that vigorous exercise does but it is possible that is may have additional, unique effects.
Hi Leigh.
I came across this comment just recently. I can see the dialogue is almost an year old but I was wondering what happened with you. I am in a similar situation and wonder if you found a solution. Thanks
I started taking natural dessicated thyroid (Naturethroid) and saw a great improvement as I gradually increased the dose, but to a limit. There’s still something going on. CT has helped some things, but not my thyroid, although I do usually forget to do it more than twice a week. (30m in 50F water is no longer a problem.)
I’m working on adding iodine (after first becoming selenium-replete) and dosing T3 two hours before I wake. I’m thinking of trying some pro-mitochondrial supp’s next (ubiquinol, d-ribose, etc.). We’ll see what happens.
Dr. Cate, I am one of those you describe perfectly – except I transitioned to VLC over about five years, starting with going from “CW healthy” to WAP/TF, and moving to primal, then eventually paleo. Still, the lower carb I go, the more I resemble what you describe.
I’m interested on your opinion on what Dr. Jack Kruse has been saying about this in the last week. It’s fascinating the timing – he is describing hibernation preparation as exactly what causes diabetes, not as a disease state,…
I adore Dr Jack Kruse (and his Quilt). But if it results from a history of poor nutrition and makes you feel sick, I’d say it’s a disease state.
So, I don’t have diabetes, or anywhere close, but as I mentioned, I went low carb very slowly over five years, and consume a 100% pastured/wild/organic diet with plenty of organ meats, broths, & ferments. No industrial foods at all. Still, my thyroid function seems to be crap.
I have no intention of returning to high, or even moderate carb intake, because it triggers binge eating in me, but I’m wondering what is going on with people like me. BTW, I’ll keep you posted on whether CT helps.
Yes, I’d be very curious. BTW, someone with your good diet could perhaps benefit from supplementation w/ either thyroid or perhaps adrenal hormone compounds if the CT and/or interval training workouts don’t fix things.
I think I may have a deeper issue. I slowly eased into a lower carb diet, first by eliminating sugars, white flour and mixed flour products, then all grains, legumes and most fruit. I started out last September, but still ate potatoes, carrots, turnips, pears and apples occasionally until January. Despite my slow transition to a pretty low carb primal diet, I still am waiting for that burst of energy promised. I am made an appt with an endocrinologist. Thanks for the post.
Keep in mind there’s a lot more to a balanced diet than cutting carbs! You also need to avoid the MegaTrans fats and get all of the Four Pillars of world cuisine into your body.
I think you missed the key word primal in my comment. I use only pastured eggs, grass fed butter, grass fed beef, pastured pork and free range chicken, only organic veggies, no commercially prepared foods whatsoever. I cannot abide liver. I eat Bubbies too! And drink occasional kombuchu and put lassi on my berries. I just do not eat bones, but I went and got some oxtails and some large bones to make stock. I hope that is enough.
I hope you can get to the root of your fatigue. All the good work you are doing to eat well will certainly assist with whatever else may be the issue.
Dr. Cate, can you please suggest a source (book or website) for good, reliable and vetted thyroid information? There seem to be laundry lists of hypo symptoms that seem to include everything under the sun. How do you sort it all out and figure out what’s normal with low carbing and what really is from hypo and needs treatment, then how to treat it? My HMO won’t even test T3 or rT3–I’m afraid to let them treat with incomplete data and approaches.
Unfortunately, most of the books I’ve encountered do not discuss the role of underlying nutritional imbalances and inflammation, and without that kind of consideration the rest of the advice falls short. So I can’t offer help with that one. I would recommend you work with a low carb doctor in your area or one of the paleo doctors from Robb Wolf’s list.
Janknitz (and Dr. Cate!)- I recommend checking out http://www.thyroidbook.com.
It’s an excellent book on the real underlying causes of hypothyroidism (whether they be autoimmune, pituitary, hormone related, etc.) Inflammation and autoimmune diet triggers are a huge part of the problem!
I’ve had really good results with my own thyroid problems using the protocols outlined in the book and a Paleo-type diet. I recommend seeking out one of the practitioners on the site.
I agree with his low-carb approach to treating the underlying cause of thyroid disease. Low carb works well for disease processes arising from inflammation, as thyroiditis is, as well as other diseases arising from hormone imbalance like PCOS, leptin resistance, infertility, weigh-loss plateaus, etc.
I’m curious….when did you switch to the Paleo camp? In Deep Nutrition, you refer to rice, pasta and sprouted bread. Now do you teach no grains at all? Have there been any studies done on the long-term effects of a grain free diet? Trying to make some decisions about how to proceed. Thanks!
Regarding the post above, one quote says, “PCOS is one kind of infertility which is reversed by low-carb diets when insulin and leptin sensitivity are reclaimed. However this will not be the case in those with severe adrenal dysfunction.” How does one know if they have “severe adrenal dysfunction”? Is there a list of doctors/naturopaths that help with these complex issues?
HI Ann
Paleo, referring to the Paleolitic era, is by definition a kind of traditional diet. It’s a little more restrictive than what I recommend, at least in the form some people describe it, but unlike adherents other diets, Paleo is not driven by any single person’s ideas, but rather by the body of science that describes what people in the past have done. Due to this built-in flexibility, Paleo is open to change. Paleo 2.0 is an example, and within Paleo there is increasing momentum toward traditional diets as a whole. If you are interested you should check out the Ancestral Health Symposium coming up this August.
If I’m reading other’s comments correctly, to correct the thyroid issues, you recommend increasing the carbs gradually…not necessarily the grains? Thanks!
Correct. Whatever form of carb you prefer.
Eating soluble fiber before the other food seems to be helping with the pain and explains why I’d have major episodes after a salad or spinach/salmon (healthy foods). My system can’t handle the insoluble fiber by itself. I hope this can help someone else. But, I hesitated to refer anyone to her site b/c her prescribed diet is low fat/no red meat/no dairy…depressing thought. Thanks again for trying to explain what’s going on with all of us who aren’t quite feeling like Mark Sisson’s gang.
Thanks for doing the research. This article gives me a lot to think about.
Good luck with your new consultation system… we newbie low carb / paleo people can use all the help we can get and you especially have been incredibly generous with answering questions. Thanks again. Best of everything.
Thanks Dr. Cate. Excellent exposition!!!
What’s missing here is the idea that all carbs are created equal. Get plenty of vegetables and you will have enough carbs. Adding back “grains” is not the solution. One would think this is common sense. Apparently not.
Fantastic. I went from a low-fat vegan diet to a “primal” diet overnight. I got very thin very fast, but could hardly move my limbs or stand for 3 minutes without stopping to lie down. One component I’m still confused about is that I also got severe joint inflammation that progressed over a period of three weeks to include every joint in my body. Got about 75% resolution of joint issues upon reintroduction of starch, but pain worsens whenever I eat legumes or red meat.
In addition to the cutting carbs too fast, there are a series of problems one can develop from adding meat too fast. One solution for some is to drink 3qts water per day and make sure you get plenty of natural salt. These all will be included in our next book.
What about an elevated ac1 level in a non-diabetic while on a long term a low carb diet – just curious. Does low carb bring about an elevated ac1 in some people as it does a rT3?
Thanks!
Do you mean A1c? Low carb brings down A1c.
🙂 While on Paleo for over a year I was experiecing the symptoms you mention in your post. Convinced I was low thyroid, I went to the doc for tests and came back with normal thyroid labs, but found a 5.9 A1c level.
Chris Kressor has had clients on paleo with high A1c levels, so the low carb has not lowered it for me; I wonder how many others may be experiencing the same issue. I thought I would ask in case you had done research in low carb and the effects on A1c as well as the thyroid.
Continuing with low carb will drop that A1c. It may have been higher before you went low carbing. Your AM fasting glucose level is also good to follow.
…getting the fuel it needs/expects, and the RT3 is turned down. They are now back to square one.
“For these people, a slow low carb might be the right thing. Switching from burning sugar to burning fat is not an easy thing to do. It is a major metabolic change.”
I’d love to hear more about your opinions on this.
Regards,
Sarabeth
Sarabeth Your friend is exactly right! In a person who has been burning carbs for decades, not getting to the point where the ever need to burn fat, there are scores of known enzymes and likely many unknown that need to be manufactured from scratch by genes that may also themselves need to be revved up again in terms of their expression.
I’d also be curious whether grain opioid withdrawal figures into the carb-flu. Perhaps easing off grains first, then attacking other carbs might be a more cautious approach? We all have heard the quip about having to eat again 10 minutes after a meal of Chinese food, but the opposite is also true.
I had the Chinese family next door over for dinner one night. We had a huge spaghetti dinner complete with salad and garlic bread (this was long before my celiac diagnosis/paleo lifestyle). Several weeks after, the wife commented she had to go home and have a bowl of rice before she felt full enough to go to bed. Perhaps she was missing her rice opioids, just like we miss our wheat opioids?
but since your insulin is still high, you are not burning fat efficiently either. So your body ‘down-regulates’ your thyroid (i.e. slows down your metabolism) to compensate. It accomplishes this by increasing production of RT3. For some people, this is a temporary condition which resolves itself as soon as the insulin resistance is overcome. But for others who are very resistant, I suspect, this condition may continue for a long time. So they eat carbs and feel better. Their body is now…
My friend had the following comment: “I suspect that the people who have problems with ‘going low carb too fast’ are precisely those who suffer the most from insulin resistance. Of course, this is only a guess, but here’s why it makes sense: If you are insulin resistant, your basal level of insulin in your blood is chronically elevated. This prevents you from releasing fat from your adipose cells to burn as fuel. So when you reduce the carbs, you reduce the fuel your body needs to function…
You are describing my low energy symptoms to a “T”. I started low carb again in late fall of last year following a stroke in Jan 2011. I’ve lost 30lbs. My neurologist ran Thyroid tests showing slightly lowered numbers for T3 and 4. He actually “prescribed” a can of caffeinated soda pop a day!
I still am fatigued. Your description is exactly how I feel.
I hope your book comes out soon because I feel I need a better-guided plan to lose the 100 lbs I must lose and return to my energetic self.
(p.s. – Android voice to text can work really well once you’ve trained it for your voice. Just a thought. http://www.makeuseof.com/tag/free-hands-speechtotext-android/ )
Hmm…
Low BP – yep, cold limbs- yep, fatigue – oh yeah. No hair loss, digestive probs all the time, on various diets, resolved by fermented live foods. No real weight probs. Fasting was sheer hell for years.
Virtual visits could be perfect for someone like me. Fill out a long form? Complete a reading list? Submit requested lab tests? THEN a live chat consult – thus a written record? That’s my M.O.
U’ve been swamped, am i right? Condense the process, i’m all 4 it. Happy to pay, not 2 waste time.
You got it. Lots of work to do on that goal, but I’m looking forward to helping more people this way.
I look forward to your new book and to meeting you in May. In the meantime, do you recommend a low GI diet with real food? Also, would a soluble fiber supplement be ok for a sluggish system? I was specifically looking at the recommendations from http://www.helpforibs.com. A low carb diet causes constipation and laxatives are a no-no. But, it sounds like regular use of a safe soluble fiber supplement can help with that and with blood sugar levels.
You could try a soluble fiber supplement for a few weeks to see if it helps. I do not find the GI to be useful in guiding my dietary advice, however.
Hi Dr Cate! What is the cause of sore muscles and stiffness from going low carb I have heard of this has lasting for 2 months, with no other symptoms. Can you discuss the muscle pain?
Lots of potential causes, which will be going into the troubleshooting section of our next book. One of the simplest is failure to hydrate.
can’t wait for the next book! any idea on the release date?
We are hoping for completion by August 2012…fingers crossed!
Hi Dr. Cate,
The bear-in-the-woods scenario you describes would absolutely mirror my experiences, except for the fact that I was eating fruit and nuts (i.e. not eating very low-carb) for a whole year before I _truly_ went “low carb” (i.e. no other carbs besides veggies and the
small amount in fermented dairy). And then it was another nine months of this supremely nutrient-dense low-carb diet before I got pregnant, which probably put a great strain on my thyroid, and was the point when I hit a wall in terms of dealing with the eight years of increasingly acute and chronic stress of raising my oldest son who is ASD.
Now my labs are showing T3 at the very bottom of the “normal” range, and my salivary cortisol is low when it should be high, and high when it should be low (and probably low overall, since it’s supposed to be much higher during pregnancy–it’s hard because I have no pre-pregnancy labs with which to compare).
But maybe in some individuals, it just takes longer to rewire things… What do you think? Another thought I’ve had, sometimes, is that maybe it’s actually a more complicated set of malfunctions that occur when a person eats a high carb diet, as I did for 30 years, without gaining weight. It sort of seems like gaining weight in such a situation is the norm, and the dysfunction that happens to people like my husband and me, who DON’T gain, almost seems more serious in some cases!! But maybe I’m just making this up.
Am very eager for your thoughts, and am very glad that you’re looking into this, because I am sure that eating more carbs is not the solution for me–I did that for 30 years, with many unfortunate consequences (even though everyone thought I was perfectly healthy because I wasn’t overweight).
I’m unclear what to do with a body that has crashed during such an “inconvenient” time as pregnancy, though. I say this while lying in bed with total fatigue and exhaustion, as I battle incredibly bizarre food revulsions as well as panic attacks and anxiety and depression that are completely debilitating. It’s making me hope that aside from completely revamping our lives in order to make them less stressful, that I can ALSO find some relief in some pharmaceutical products that I have never ever wanted to use before in my life…
I haven’t come up with any solutions for my situation at this acute and timely stage…besides cortisol and thyroid meds. I have only this week found a doctor who feels confident to prescribe during pregnancy (although everyone and their second cousin could have prescribed psychiatric meds to me months ago!), and at this point, I feel like I have no other options. I am dying for relief.
Regards,
Sarabeth
Sarabeth, it’s common to develop autoimmune thyroid disease during pregnancy or postpartum:
http://functionalhealthnews.com/2012/02/hypothyroidism-during-pregnancy-more-common-than-thought/
I’d get a full thyroid panel, including an antibody panel and refer to the functional medicine lab ranges outlined in the book http://www.thyroidbook.com to interpret your results (or even better, start working with a functional medicine practitioner:)
Wow, this describes me to a T!!! I have belieced, for years, that starchy carbs/sugars, are most likely the roit of my lifelong digestive issues (and chronic yeast/bacterial) overgrowth, and have tried MANY times over the years to get off them only to return because I just feel worse being off! And I have given my body a long period if time to adjust but I never seem to pull out of feeling bad! Symptoms are always the same – chronic fatigue, LOW blood pressure (averaging 85/53) heavy fatigue (you pegged it when you saud the overwhelming feeling if wanting to hibernate – I just get shut down mentally and feel NO motivationor umph to do ANYTHING) and overwhelming cravings for anything starchy! I have attributed to emotional addiction, which I believe is there, but I can just FEEL a deep body NEED fir them that I’d beyond me. And as soon as I go back on them, allif those symptoms life to a large degree but then I get hit w the other digestive, joint and headache type symptoms! So I have been doing thus crazy cycling exchanging one set of symptoms for another for years and SO WEARY if it all. Know too, that I have developed a real negative feel toward food that I’d nit healthy as well because it’s always caused me such agony!
Question- any advice as to how long to slowly go off the carbs and the safest carbs to eat during the weaning process? Also would be very interested in setting up a phone consult w you to discuss this all further. I read your Deep Nutrition book and lived all your wonderful, in depth information. I have a nutrition practice here in Oahu (not active now as much due to health) we actually moved here from Seattle to this Warner climate for my health because I was always SO cold – lived hovering over my heater (as I was hibernating!)
The other tough issue I have in going off the carbs is that I don’t tolerate/digest meats/fish or nuts/seeds so I am left mainly w veggies and fruit. I am already on the thin side and really can’t afford to lose any more weight. Just feel So STUCK between a rock and a hard place!!!
Would love your input!! Desperate for help at this point!!
Mahalo and blessings!
Sue Fowler
Thehealingpath@aol.com
Pardon the spelling errors – typed on my little iPhone keyboard!
I’d love to work out a plan for you once I’ve got the phone consultation available. In the meantime, you may want to begin weaning by identifying your most addictive (ie favorite) sweet/starchy food and work on cutting that down by half and then to 10% over the next month.
Please let me know as soon as you are available for the phone consults (or better yet Skype?? ; ) I will try doing as you advised, thanks for the info ! God bless!
I promise to do a post about it so that subscribers to my RSS feed will be notified!
You may paste this into your browser to subscribe: http://feeds2.feedburner.com/drcate/PBhs
Dr. Cate – what do you think of Matt Stone’s latest discussions, specifically his rallying against low carb eating? Here’s a post where he talks about starch and insulin levels: http://180degreehealth.com/2011/06/starch-lowers-insulin
I don’t follow his logic.
I don’t feel badly but I do have digestion problems (bloating, constipation, etc.). I am cold and lose a lot of hair. I have never dieted at all. In fact, I was attracted to your books because they seemed to describe a healthy lifestyle for all people…not just the overweight. Nonetheless, after six months, something isn’t working quite right. Do you recommend adding back grains specifically or just more carbs in general (fruit, squash, potatoes, etc.)? I’d like to keep my blood sugar in check and of course not gain back the 10 pounds I lost initially. By the way, my T4 Free is 1.1, TSH is 1.88 and T3 Reverse is 31. Thanks for writing this. I so appreciate having things explained medically otherwise we’d just assume paleo was anther fad diet. We’re looking for a healthy lifestyle for the long-term not a quick fix diet.
Hmmm. Without more info I would not want to misadvise you. We would need to take a closer look at your diet and other lab numbers. At the risk of sounding like a salesperson, starting in May I am going to be doing virtual visits in order to be able to help folks like you work through these metabolic glitches as quickly and safely as possible.